Wed, May 6, 2026
| فارسی
Volume 28, Issue 4 (Winter 2023)
IJPCP 2023, 28(4): 478-491 |
Back to browse issues page
Download citation:
BibTeX | RIS | EndNote | Medlars | ProCite | Reference Manager | RefWorks
Send citation to:



BibTeX | RIS | EndNote | Medlars | ProCite | Reference Manager | RefWorks
Send citation to:
Nazari F, Gharraee B, Zahedi Tajrishi K. Mediating role of Emotion Dysregulation, Experiential Avoidance, and Rumination in the Relationship of Emotional Schemas with Obsessive-Compulsive Disorder Symptoms. IJPCP 2023; 28 (4) :478-491
URL: http://ijpcp.iums.ac.ir/article-1-3860-en.html
URL: http://ijpcp.iums.ac.ir/article-1-3860-en.html
1- Department of Clinical Psychology, School of Behavioral Sciences and Mental Health (Tehran Institute of Psychiatry), Iran University of Medical Sciences, Tehran, Iran.
2- Department of Clinical Psychology, School of Behavioral Sciences and Mental Health (Tehran Institute of Psychiatry), Iran University of Medical Sciences, Tehran, Iran. ,gharaee.b@iums.ac.ir
2- Department of Clinical Psychology, School of Behavioral Sciences and Mental Health (Tehran Institute of Psychiatry), Iran University of Medical Sciences, Tehran, Iran. ,
Keywords: Emotion dysregulation, Emotional schemas, Rumination, Experiential avoidance, Obsessive-compulsive disorder
Full-Text [PDF 6287 kb]
(1474 Downloads)
| Abstract (HTML) (3299 Views)
Full-Text: (2158 Views)
Introduction
Obsessive-compulsive disorder (OCD) is characterized by unwanted thoughts, images or tendencies (obsessions), which are followed by repetitive behaviors or mental acts (compulsions) experienced in response to anxiety or other unfavorable emotions [1]. Obsessive-compulsive symptoms (OCSs) usually occur in a non-clinical, subclinical, and clinical continuum that differ in the severity of cognition and symptoms, but they are qualitatively identical in nature. Thus, most of the subclinical OCSs may progress to OCD, if left untreated [2]. Epidemiological studies in the United States report that about 28.2% of people in the community have experienced OCSs at least once in their lifetime [4]. Furthermore, according to an epidemiological study in Iran, the prevalence of OCS among adolescents was found as 11.2% [5]. Defective emotional schemas are associated with OCSs [5]. The emotional schema model states that individuals have different perspectives about emotion and emotion regulation, which cause problematic strategies to cope with emotions, such as suppression, rumination, avoidance, blaming, and substance abuse [10]. Emotion regulation is defined by Gross as: “the processes, by which individuals influence which emotions they have, when they have them, and how they experience and express these emotions” [12]. Moreover, it seems that defective emotion regulation may be associated with a growth in repetitive efforts to avoid emotional experiences [13]. Thus, experiential avoidance (EA) may play a key role in the formation and persistence of a number of mental health-related disorders, like anxiety, depression, and OCD [14]. In addition, interest in understanding the cognitive processes involved in the pathology of OCD has increased in recent years. One of the cognitive factors that has attracted little attention is rumination. It is believed that rumination may aggravate the OCSs [17].
To the best of the author’s knowledge, a study examining the mediating role of emotion dysregulation, rumination, and experiential avoidance in the relationship between OCSs and emotional schemas has not yet been done. Thus, this study was designed to examine a more comprehensive model of OCSs.
Methods
This is a descriptive-correlational study, which was done using the structural equation modeling method (SEM). The Sobel test was used to evaluate the mediating role of emotion dysregulation, experiential avoidance, and rumination. The sample included 349 students selected by convenience sampling from the universities of Tehran. The inclusion criteria were being a college student and the age of 20-40 years. Further, participants were excluded if they had psychosis, bipolar disorders, post-traumatic stress disorder (assessed by self-declaration) as well as substance use disorder (assessed by questionnaire). Due to the COVID-19 outbreak, the data collection process was done online. The Obsessive Compulsive Inventory-Revised (OCI-R), Leahy’s Emotional Schemas Questionnaire (LESS), Difficulty in Emotion Regulation Scale (DERS), The Ruminative Response Scale, Acceptance, and Action Questionnaire-II (AAQ-II), and Drug Use Disorders Identification Test (DUDIT) were used to collect the data.
Results
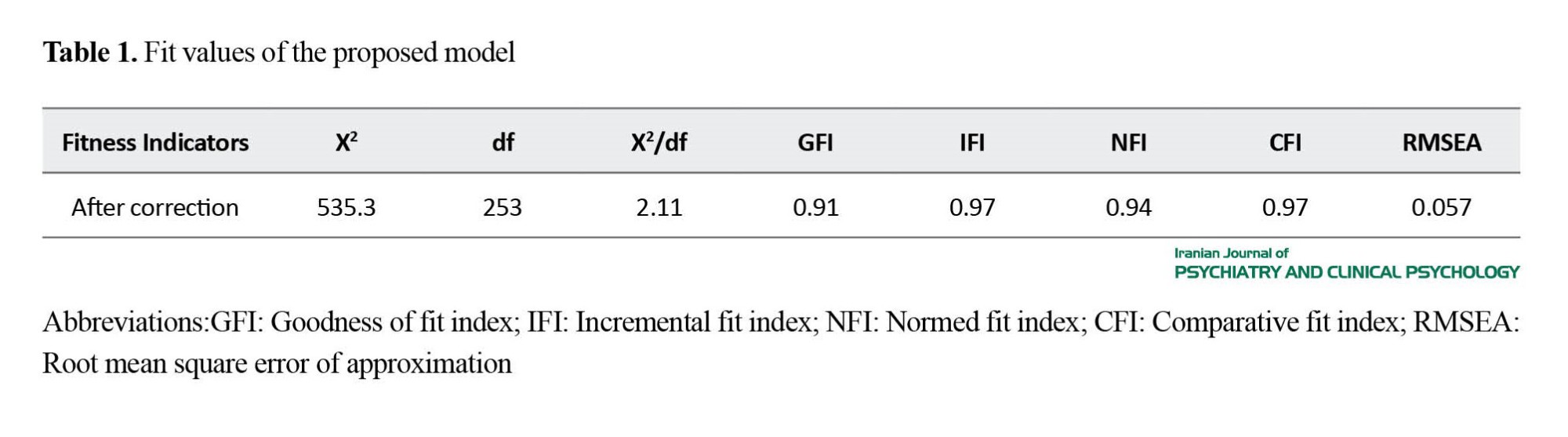
According to the fit values, the proposed model had a good fit (Table 1). Moreover, the Sobel test was used to investigate the mediating role of emotional dysregulation, rumination, and experiential avoidance in the relationship between emotional schemas and OCSs. Considering that at the error level of 0.05 (α=0.05) and the significance level of less than 0.05 for all of these three variables, it can be said that their mediating role was statistically significant.
Discussion
The results show that the relationship between emotional schemas and OCSs via emotion dysregulation was statistically significant. Consistent with this result, Stern et al. found that the anxiety associated with OCSs is significantly associated with low emotional awareness and fear of positive and negative emotions [38]. In addition, in explaining the present findings, we can also refer to Leahy’s emotional schema model. This model states that negative beliefs about emotions lead to the use of ineffective strategies to deal with them. As a result, if a person has some negative beliefs about their emotions, they will use dysfunctional emotion regulation strategies, such as avoidance and repression, which in this case, obsessions can be considered a way to suppress and avoid the experiencing of emotions [8]. Furthermore, findings showed that rumination is a significant mediator of the relationship between emotional schemas and OCSs. Individuals who do not believe that their emotions are considered valid by others and that their emotions are not understandable to them have low acceptance of their emotions and are more likely to ruminate [8] and this rumination can be the basis of obsessive thoughts and behaviors.
About the mediating role of experiential avoidance (, we can refer to the findings of Rezaei et al. [20], Angelakis et al. [4], and Briggs et al. [45].
Leahy et al. [46] also showed that maladaptive emotional schemas have a positive and significant correlation with experiential avoidance and can significantly predict it. Leahy believes that adaptive emotional schemas lead to a moment-by-moment increase in mindfulness (reduced experiential avoidance), acceptance, and experience of emotions [44]. In addition, it can be stated that experiential avoidance plays a key role in the formation and continuation of OCD. Considering that the prevalence of intrusive thoughts in people with OCD is not more than in the general population, probably the meaning that the first group gives to these thoughts and then avoids their experience is the basis for the formation of symptoms. The present study highlights the important role of emotion dysregulation, experiential avoidance, rumination, and emotional schemas in the formation of OCSs. However, the interpretation of findings must be considered along with the study’s limitations. For example, due to the prevalence of COVID-19 and the closure of universities, it was not possible to conduct the data collection process in person and select participants randomly. Therefore, the convenience sampling method was inevitably used and the data were collected online. Furthermore, the sample was non-clinical; thus, it can make it complicated to generalize the findings of this study to clinical and subclinical groups. Future studies would benefit from incorporating participants with a diagnosis of OCD based on a structured clinical interview for DSM-5.
Ethical Considerations
Compliance with ethical guidelines
The present study was approved by the ethics committee of Iran University of Medical Sciences (Code: IR.IUMS.REC.1400.294).
Funding
This study was extracted from the MSc thesis of Fatemeh Nazari, approved by Iran University of Medical Sciences. The authors received no financial support for research..
Authors contributions
Conceptualization, project administration, research, writing original draft, review, validation: Fatemeh Nazari; Conceptualization, validation, supervision, writing, review and editing: Banafshe Gharaee; Methodology, formal analysis and editing: Komeil Zahedi Tajrishi.
Conflicts of interest
The authors declared no conflict of interest.
Obsessive-compulsive disorder (OCD) is characterized by unwanted thoughts, images or tendencies (obsessions), which are followed by repetitive behaviors or mental acts (compulsions) experienced in response to anxiety or other unfavorable emotions [1]. Obsessive-compulsive symptoms (OCSs) usually occur in a non-clinical, subclinical, and clinical continuum that differ in the severity of cognition and symptoms, but they are qualitatively identical in nature. Thus, most of the subclinical OCSs may progress to OCD, if left untreated [2]. Epidemiological studies in the United States report that about 28.2% of people in the community have experienced OCSs at least once in their lifetime [4]. Furthermore, according to an epidemiological study in Iran, the prevalence of OCS among adolescents was found as 11.2% [5]. Defective emotional schemas are associated with OCSs [5]. The emotional schema model states that individuals have different perspectives about emotion and emotion regulation, which cause problematic strategies to cope with emotions, such as suppression, rumination, avoidance, blaming, and substance abuse [10]. Emotion regulation is defined by Gross as: “the processes, by which individuals influence which emotions they have, when they have them, and how they experience and express these emotions” [12]. Moreover, it seems that defective emotion regulation may be associated with a growth in repetitive efforts to avoid emotional experiences [13]. Thus, experiential avoidance (EA) may play a key role in the formation and persistence of a number of mental health-related disorders, like anxiety, depression, and OCD [14]. In addition, interest in understanding the cognitive processes involved in the pathology of OCD has increased in recent years. One of the cognitive factors that has attracted little attention is rumination. It is believed that rumination may aggravate the OCSs [17].
To the best of the author’s knowledge, a study examining the mediating role of emotion dysregulation, rumination, and experiential avoidance in the relationship between OCSs and emotional schemas has not yet been done. Thus, this study was designed to examine a more comprehensive model of OCSs.
Methods
This is a descriptive-correlational study, which was done using the structural equation modeling method (SEM). The Sobel test was used to evaluate the mediating role of emotion dysregulation, experiential avoidance, and rumination. The sample included 349 students selected by convenience sampling from the universities of Tehran. The inclusion criteria were being a college student and the age of 20-40 years. Further, participants were excluded if they had psychosis, bipolar disorders, post-traumatic stress disorder (assessed by self-declaration) as well as substance use disorder (assessed by questionnaire). Due to the COVID-19 outbreak, the data collection process was done online. The Obsessive Compulsive Inventory-Revised (OCI-R), Leahy’s Emotional Schemas Questionnaire (LESS), Difficulty in Emotion Regulation Scale (DERS), The Ruminative Response Scale, Acceptance, and Action Questionnaire-II (AAQ-II), and Drug Use Disorders Identification Test (DUDIT) were used to collect the data.
Results
According to the fit values, the proposed model had a good fit (Table 1). Moreover, the Sobel test was used to investigate the mediating role of emotional dysregulation, rumination, and experiential avoidance in the relationship between emotional schemas and OCSs. Considering that at the error level of 0.05 (α=0.05) and the significance level of less than 0.05 for all of these three variables, it can be said that their mediating role was statistically significant.

Discussion
The results show that the relationship between emotional schemas and OCSs via emotion dysregulation was statistically significant. Consistent with this result, Stern et al. found that the anxiety associated with OCSs is significantly associated with low emotional awareness and fear of positive and negative emotions [38]. In addition, in explaining the present findings, we can also refer to Leahy’s emotional schema model. This model states that negative beliefs about emotions lead to the use of ineffective strategies to deal with them. As a result, if a person has some negative beliefs about their emotions, they will use dysfunctional emotion regulation strategies, such as avoidance and repression, which in this case, obsessions can be considered a way to suppress and avoid the experiencing of emotions [8]. Furthermore, findings showed that rumination is a significant mediator of the relationship between emotional schemas and OCSs. Individuals who do not believe that their emotions are considered valid by others and that their emotions are not understandable to them have low acceptance of their emotions and are more likely to ruminate [8] and this rumination can be the basis of obsessive thoughts and behaviors.
About the mediating role of experiential avoidance (, we can refer to the findings of Rezaei et al. [20], Angelakis et al. [4], and Briggs et al. [45].
Leahy et al. [46] also showed that maladaptive emotional schemas have a positive and significant correlation with experiential avoidance and can significantly predict it. Leahy believes that adaptive emotional schemas lead to a moment-by-moment increase in mindfulness (reduced experiential avoidance), acceptance, and experience of emotions [44]. In addition, it can be stated that experiential avoidance plays a key role in the formation and continuation of OCD. Considering that the prevalence of intrusive thoughts in people with OCD is not more than in the general population, probably the meaning that the first group gives to these thoughts and then avoids their experience is the basis for the formation of symptoms. The present study highlights the important role of emotion dysregulation, experiential avoidance, rumination, and emotional schemas in the formation of OCSs. However, the interpretation of findings must be considered along with the study’s limitations. For example, due to the prevalence of COVID-19 and the closure of universities, it was not possible to conduct the data collection process in person and select participants randomly. Therefore, the convenience sampling method was inevitably used and the data were collected online. Furthermore, the sample was non-clinical; thus, it can make it complicated to generalize the findings of this study to clinical and subclinical groups. Future studies would benefit from incorporating participants with a diagnosis of OCD based on a structured clinical interview for DSM-5.
Ethical Considerations
Compliance with ethical guidelines
The present study was approved by the ethics committee of Iran University of Medical Sciences (Code: IR.IUMS.REC.1400.294).
Funding
This study was extracted from the MSc thesis of Fatemeh Nazari, approved by Iran University of Medical Sciences. The authors received no financial support for research..
Authors contributions
Conceptualization, project administration, research, writing original draft, review, validation: Fatemeh Nazari; Conceptualization, validation, supervision, writing, review and editing: Banafshe Gharaee; Methodology, formal analysis and editing: Komeil Zahedi Tajrishi.
Conflicts of interest
The authors declared no conflict of interest.
References:
- Nissen JB, Højgaard DRMA, Thomsen PH. The immediate effect of COVID-19 pandemic on children and adolescents with obsessive compulsive disorder. BMC Psychiatry. 2020; 20(1):511. [DOI:10.1186/s12888-020-02905-5] [PMID] [PMCID]
- Adams TG, Kelmendi B, Brake CA, Gruner P, Badour CL, Pittenger C. The role of stress in the pathogenesis and maintenance of obsessive-compulsive disorder. Chronic Stress. 2018; 2:2470547018758043. [DOI:10.1177/2470547018758043] [PMID] [PMCID]
- Ahowan M, Jajarmi M, Bakhshipoor A. [Comparing the effectiveness of schema therapy (ST) and emotional schema therapy (EST) on clinical syndromes of individuals with obsessive-compulsive symptoms (OCS) (Persian)]. Avicenna Journal of Nursing and Midwifery Care. 2020; 28(3):239-50. [DOI:10.30699/ajnmc.28.3.239]
- Angelakis I, Pseftogianni F. Association between obsessive-compulsive and related disorders and experiential avoidance: A systematic review and meta-analysis. Journal of Psychiatric Research. 2021; 138:228-39. [DOI:10.1016/j.jpsychires.2021.03.062] [PMID]
- Shams G, Foroughi E, Esmaili Y, Amini H, Ebrahimkhani N. Prevalence rates of obsessive-compulsive symptoms and psychiatric comorbidity among adolescents in Iran. Acta Medica Iranica. 2011; 49(10):680-7. [PMID]
- Zare MM, Bagooli H, Kazemi SA, Javidi HA. [Comparison of emotional schemes in war veterans suffering post traumatic stress disorder with depression symptoms, anxiety symptoms and without signs of depression and anxiety (Persian)]. Iranian Journal of War and Public Health. 2020; 12(1):53-61. [DOI:10.29252/ijwph.12.1.53]
- Khosravani V, Samimi Ardestani SM, Mohammadzadeh A, Sharifi Bastan F, Amirinezhad A. The emotional schemas and obsessive-compulsive symptom dimensions in people with obsessive-compulsive disorder. International Journal of Cognitive Therapy. 2020; 13:341-57. [DOI:10.1007/s41811-020-00075-6]
- Leahy RL. A model of emotional schemas. Cognitive and Behavioral Practice. 2002; 9(3):177-90. [DOI:10.1016/S1077-7229(02)80048-7]
- Leahy RL. Emotional schema therapy: A meta-experiential model. Australian Psychologist. 2016; 51(2):82-8. [DOI:10.1111/ap.12142]
- Leahy RL. Introduction: Emotional schemas, emotion regulation, and psychopathology. International Journal of Cognitive Therapy. 2012; 5(4):359-61. [DOI:10.1521/ijct.2012.5.4.359]
- Cisler JM, Olatunji BO. Emotion regulation and anxiety disorders. Current Psychiatry Reports. 2012; 14(3):182-7. [DOI:10.1007/s11920-012-0262-2] [PMID] [PMCID]
- Gross JJ. The emerging field of emotion regulation: An integrative review. Review of General Psychology. 1998; 2(3):271-99. [DOI:10.1037/1089-2680.2.3.271]
- Stern MR, Nota JA, Heimberg RG, Holaway RM, Coles ME. An initial examination of emotion regulation and obsessive compulsive symptoms. Journal of Obsessive-Compulsive and Related Disorders. 2014; 3(2):109-14. [DOI:10.1016/j.jocrd.2014.02.005]
- Angelakis I, Gooding P. Obsessive-compulsive disorder and suicidal experiences: The role of experiential avoidance. Suicide & Life-Threatening Behavior. 2020; 50(2):359-71. [DOI:10.1111/sltb.12593] [PMID]
- Abramowitz JS, Lackey GR, Wheaton MG. Obsessive-compulsive symptoms: The contribution of obsessional beliefs and experiential avoidance. Journal of Anxiety Disorders. 2009; 23(2):160-6.[DOI:10.1016/j.janxdis.2008.06.003] [PMID]
- Mardani A, Alimohammadi A, Mahmoudi Tabar M. [The structural relationship between emotional schemas and experiential avoidance with self-harm behaviors: The mediating role of smartphone addiction (Persian)]. Rooyesh-e-Ravanshenasi Journal. 2022; 11(7):145-54. [Link]
- Raines A, Vidaurri DN, Portero AK, Schmidt NB. Associations between rumination and obsessive-compulsive symptom dimensions. Personality and Individual Differences. 2017; 113:63-7. [DOI:10.1016/j.paid.2017.03.001]
- Watkins E, Brown RG. Rumination and executive function in depression: an experimental study. Journal of Neurology, Neurosurgery, and Psychiatry. 2002; 72(3):400-2. [DOI:10.1136/jnnp.72.3.400] [PMID] [PMCID]
- Lyubomirsky S, Kasri F, Chang O, Chung I. Ruminative response styles and delay of seeking diagnosis for breast cancer symptoms. Journal of Social and Clinical Psychology. 2006; 25(3):276-304. [DOI:10.1521/jscp.2006.25.3.276]
- Rezaei M, Ghazanfari F, Rezaee F. The role of childhood trauma, early maladaptive schemas, emotional schemas and experimental avoidance on depression: A structural equation modeling. Psychiatry Research. 2016; 246:407-14. [DOI:10.1016/j.psychres.2016.10.037] [PMID]
- Huz I, Nyer M, Dickson C, Farabaugh A, Alpert J, Fava M, et al. Obsessive-compulsive symptoms as a risk factor for suicidality in U.S. college students. The Journal of Adolescent Health. 2016; 58(4):481-4. [DOI:10.1016/j.jadohealth.2015.11.011] [PMID]
- Assareh M, Rakhshani T, Kashfi M, Ayazi M. Status of obsessive compulsive disorder among Iranian college students in Kermanshah, Iran. Journal of Human, Environment and Health Promotion. 2016; 1(4):213-9. [DOI:10.29252/jhehp.1.4.213]
- Foa EB, Huppert JD, Leiberg S, Langner R, Kichic R, Hajcak G, et al. The obsessive-compulsive inventory: Development and validation of a short version. Psychological Assessment. 2002; 14(4):485-96. [DOI:10.1037/1040-3590.14.4.485] [PMID]
- Mohammadi AAF, Zamani R, Fata L. [Validation of the persian version of the obsessive-compulsive inventory-revised in a student sample (Persian)]. Psychological Research. 2008;11(1-2):66-78. [Link]
- Fergus TA, Bardeen JR. Emotion regulation and obsessive-compulsive symptoms: A further examination of associations. Journal of Obsessive-Compulsive and Related Disorders. 2014; 3(3):243-8. [DOI:10.1016/j.jocrd.2014.06.001]
- Gratz KL, Roemer L. Multidimensional assessment of emotion regulation and dysregulation: Development, factor structure, and initial validation of the difficulties in emotion regulation scale. Journal of Psychopathology and Behavioral Assessment. 2004; 26:41-54. [DOI:10.1023/B:JOBA.0000007455.08539.94]
- Khanzadeh M, Saeediyan M, Hosseinchari M, Edrissi F. Factor structure and psychometric properties of difficulties in emotional regulation scale. International Journal of Behavioral Sciences. 2012; 6(1):87-96. [Link]
- Mousavi E, Gharraee B, Ramazani Farani A, Taremian F. [Comparison of cognitive errors and rumination in obsessive-compulsive and social phobia disorders (Persian)]. Iranian Journal of Psychiatry and Clinical Psychology. 2017; 23(1):10-21. [DOI:10.18869/nirp.ijpcp.23.1.10]
- Roelofs J, Muris P, Huibers M, Peeters F, Arntz A. On the measurement of rumination: A psychometric evaluation of the ruminative response scale and the rumination on sadness scale in undergraduates. Journal of Behavior Therapy and Experimental Psychiatry. 2006; 37(4):299-313. [DOI:10.1016/j.jbtep.2006.03.002] [PMID]
- Farnam A , Bakhshipour Roodsari A, Mansouri A, Mahmood Aliloo M. [The comparison of rumination in patients with major depression disorder, obsessive-compulsive disorder, generalized anxiety disorder and normal individuals (Persian)]. Journal of Sabzevar University of Medical Sciences, 1970; 17(3):189-95. [Link]
- Asadi S, Abedini M, Poursharifi H, Nikokar M. [The relationship between intolerance of uncertainty and rumination with worry on student population (Persian)]. Journal of Clinical Psychology. 2012; 4(4):83-92. [DOI:10.22075/JCP.2017.2110
- Jenadeleh K, Bassak Nejad S, Yunesi A, Sadatmand K. [The relationship between anxiety sensitivity and experiential avoidance and resiliency with test anxiety in male students (Persian)]. Journal of Clinical Psychology. 2018; 10(1):71-8. [DOI:10.22075/JCP.2018.13974.1361]
- Moradi Kelardeh S, Aghajani S, Ghasemi Jobaneh R, Baharvand I. [Role of integrative self-knowledge, experiential avoidance and self-compassion in test anxiety of female students (Persian)]. Education Strategies Medical Sciences. 2019; 12(1):110-5. [DOI:10.29252/edcbmj.12.01.15]
- Reuman L, Buchholz J, Abramowitz JS. Obsessive beliefs, experiential avoidance, and cognitive fusion as predictors of obsessive-compulsive disorder symptom dimensions. Journal of Contextual Behavioral Science. 2018; 9:15-20. [DOI:10.1016/j.jcbs.2018.06.001]
- Abasi E, Fti L, Molodi R, Zarabi H. [Psychometric properties of Persian version of acceptance and action questionnaire -II (Persian)]. Psychological Methods and Models. 2013; 3-2(10):65-80. [Link]
- Habibi M, Alahdadi S, Salari M, Ghanbari N. [Psychometric properties of drug use disorders identification test (DUDIT) among drug abusers (Persian)]. Iranian Journal of Epidemiology. 2017; 13(3):210-21. [Link]
- Berman AH, Bergman H, Palmstierna T, Schlyter F. Evaluation of the drug use disorders identification test (DUDIT) in criminal justice and detoxification settings and in a Swedish population sample. European Addiction Research. 2005; 11(1):22-31.[DOI:10.1159/000081413] [PMID]
- Faustino B, Vasco AB. Emotional schemas mediate the relationship between emotion regulation and symptomatology. Current Psychology. 2021; 42:2733-9. [DOI:10.1007/s12144-021-01560-7]
- Alikhani Z, Amirimajd M. [The relationship components of meta-worry, rumination and psychological flexibility with obsessive-compulsive spectrum disorders (Persian)]. Journal of Thought & Behavior in Clinical Psychology. 2019; 14(52):47-56. [Link]
- Rezaee M, Ghazanfari F, Rezaee F. [Effectiveness of emotional schema therapy on severity of depression and rumination in people with major depressive disorder (Persian)]. Journal of Shahid Sadoughi University of Medical Sciences. 2016; 24(1):41-56. [Link]
- Mohammadi H, Sepehri Shamlou Z, Asghari Ebrahim Abad MJ. [The effectiveness of group emotional schema therapy on decreasing loneliness and rumination in divorced women (Persian)]. Journal of Woman and Family Studies. 2019; 7(2):115-36. [DOI:10.22051/JWFS.2020.19718.1708]
- Wahl K, Ertle A, Bohne A, Zurowski B, Kordon A. Relations between a ruminative thinking style and obsessive-compulsive symptoms in non-clinical samples. Anxiety, Stress, and Coping. 2011; 24(2):217-25. [DOI:10.1080/10615806.2010.482985] [PMID]
- Abramowitz JS, Taylor S, McKay D. Obsessive-compulsive disorder. Lancet. 2009; 374(9688):491-9. [DOI:10.1016/S0140-6736(09)60240-3] [PMID]
- Freeston MH, Ladouceur R. What do patients do with their obsessive thoughts? Behaviour Research and Therapy. 1997; 35(4):335-48. [DOI:10.1016/S0005-7967(96)00094-0] [PMID]
- Briggs ES, Price IR. The relationship between adverse childhood experience and obsessive-compulsive symptoms and beliefs: The role of anxiety, depression, and experiential avoidance. Journal of Anxiety Disorders. 2009; 23(8):1037-46. [DOI:10.1016/j.janxdis.2009.07.004] [PMID]
- Leahy RL, Tirch DD, Melwani PS. Processes underlying depression: Risk aversion, emotional schemas, and psychological flexibility. International Journal of Cognitive Therapy. 2012; 5(4):362-79. [DOI:10.1521/ijct.2012.5.4.362]
- Oguz G, Celikbas Z, Batmaz S, Cagli S, Sungur MZ. Comparison between obsessive compulsive disorder and panic disorder on metacognitive beliefs, emotional schemas, and cognitive flexibility. International Journal of Cognitive Therapy. 2019; 12(3):157-78. [DOI:10.1007/s41811-019-00047-5]
- Edwards ER, Liu Y, Ruiz D, Brosowsky NP, Wupperman P. Maladaptive emotional schemas and emotional functioning: Evaluation of an integrated model across two independent samples. Journal of Rational-Emotive and Cognitive-Behavior Therapy. 2020; 39:428-55. [DOI:10.1007/s10942-020-00379-8]
- Heinzel CV, Kollárik M, Miché M, Clamor A, Ertle A, Lieb R, et al. Is a ruminative thinking style related to obsessive-compulsive symptom severity beyond its associations with depressive and anxiety symptom severity? International Journal of Cognitive Therapy. 2021; 14:575-91. [DOI:10.1007/s41811-021-00112-y]
Type of Study: Original Research |
Subject:
Psychiatry and Psychology
Received: 2023/02/23 | Accepted: 2023/04/17 | Published: 2023/01/1
Received: 2023/02/23 | Accepted: 2023/04/17 | Published: 2023/01/1
| Rights and permissions | |
 |
This work is licensed under a Creative Commons Attribution-NonCommercial 4.0 International License. |






