Mon, Apr 27, 2026
| فارسی
Volume 31, Issue 1 (Continuously Updated 2025)
IJPCP 2025, 31(1): 0-0 |
Back to browse issues page
Download citation:
BibTeX | RIS | EndNote | Medlars | ProCite | Reference Manager | RefWorks
Send citation to:



BibTeX | RIS | EndNote | Medlars | ProCite | Reference Manager | RefWorks
Send citation to:
Dehghani F, Salehzadeh M, Bakhshayesh A, Dastjerdi G. Comparing the Quality of Interpersonal Relationships in Individuals With and Without Obsessive-Compulsive Disorder: Excessive Reassurance Seeking and Perceived Interpersonal Relationships. IJPCP 2025; 31 (1)
URL: http://ijpcp.iums.ac.ir/article-1-4287-en.html
URL: http://ijpcp.iums.ac.ir/article-1-4287-en.html
1- Department of Psychology, Faculty of Psychology and Educational Sciences, Yazd University, Yazd, Iran.
2- Department of Psychology, Faculty of Psychology and Educational Sciences, Yazd University, Yazd, Iran. ,m.salehzadeh@yazd.ac.ir
3- Department of Psychiatry, Faculty of Medicine, Shahid Sadoughi University of Medical Sciences, Yazd, Iran.
2- Department of Psychology, Faculty of Psychology and Educational Sciences, Yazd University, Yazd, Iran. ,
3- Department of Psychiatry, Faculty of Medicine, Shahid Sadoughi University of Medical Sciences, Yazd, Iran.
Full-Text [PDF 6249 kb]
(661 Downloads)
| Abstract (HTML) (1117 Views)
Full-Text: (101 Views)
Introduction
Obsessive-Compulsive disorder (OCD) is characterized by disturbing, intrusive, anxiety-provoking thoughts (obsessions) and or repetitive behavior (compulsions) [1، 2]. Persistent suspicion or concern about threats or potential harm can prompt people to constantly ask others for information and opinions [3، 7]. This behavior is known as excessive reassurance seeking (ERS) [9]. When reassurance-seeking becomes pervasive in OCD, it can have significant effects on interpersonal relationships [15]. Individuals with OCD often rely on family members and friends. The relatives and caregivers of individuals with OCD are frequently involved in providing reassurance because the families of these individuals are likely to contribute to the symptoms of OCD. This accommodation (ie, assuring) is mostly due to the fact that the symptoms of OCD often and mainly occur at home [17].
Caregivers of individuals with OCD state that persistent reassurance has negative effects on their relations and induces feelings of frustration, anger, and sometimes guilt [16]. In general, the results of previous studies on the interpersonal effects of reassurance-seeking are different and sometimes inconsistent. Halldorsson et al. [16] and Kobori et al. [26] showed that reassurance triggers frustration in caregivers, while Halldorsson and Salkovskis [11] referred to the positive effect of excessive reassurance-seeking (ERS) on interpersonal relationships. Tetelman [17] also reported a positive association between accommodation and relationship satisfaction. In this regard, this research aims to compare the perceived quality of interpersonal relationships in individuals with OCD and a healthy group and investigate the relationship between ERS and the perceived quality of interpersonal relationships in individuals with OCD.
Methods
This study was descriptive and causal-comparative. The statistical population consisted of individuals with OCD who referred to medical centers in Yazd City, Iran, in the fall of 2018 and healthy individuals. In this study, based on the Cochran formula, 102 individuals with OCD and 102 individuals without OCD were selected through purposive sampling. The OCD cases were invited to participate in this study by the psychiatric ward of three medical centers affiliated with Yazd University of Medical Sciences. The inclusion criteria for OCD group were as follows: a) Literacy, b) Absence of other psychiatric disorders based on clinical interviews by a psychiatrist, such as mood disorders, ie, bipolar mood disorder and depression, psychotic disorders, obsessive-compulsive personality disorder and other personality abnormalities, c) Absence of serious medical diseases such as diabetes, Parkinson and neurological diseases like MS, and d) Lack of drug abuse. Trained psychiatrists of Yazd University of Medical Sciences selected the OCD group. Individuals without OCD were chosen in terms of demographic variables corresponding to the OCD group. In addition, the criterion for opting the individuals without OCD to participate in the study was no history of psychiatric diagnosis, clinical complaint, or use of psychiatric drugs. Yale-Brown obsessive-compulsive scale (Y-BOCS) and reassurance seeking questionnaire (ReSQ) (This questionnaire comprises four scales: Source, trust, intensity, and carefulness) were completed by individuals with OCD. Pierce quality of relationship inventory (QRI) (This questionnaire comprises three scales: social support, interpersonal conflicts, and depth of relationship) was completed by both groups, and the data were analyzed using the Pearson correlation and multivariate analysis of variance (MANOVA).
Results
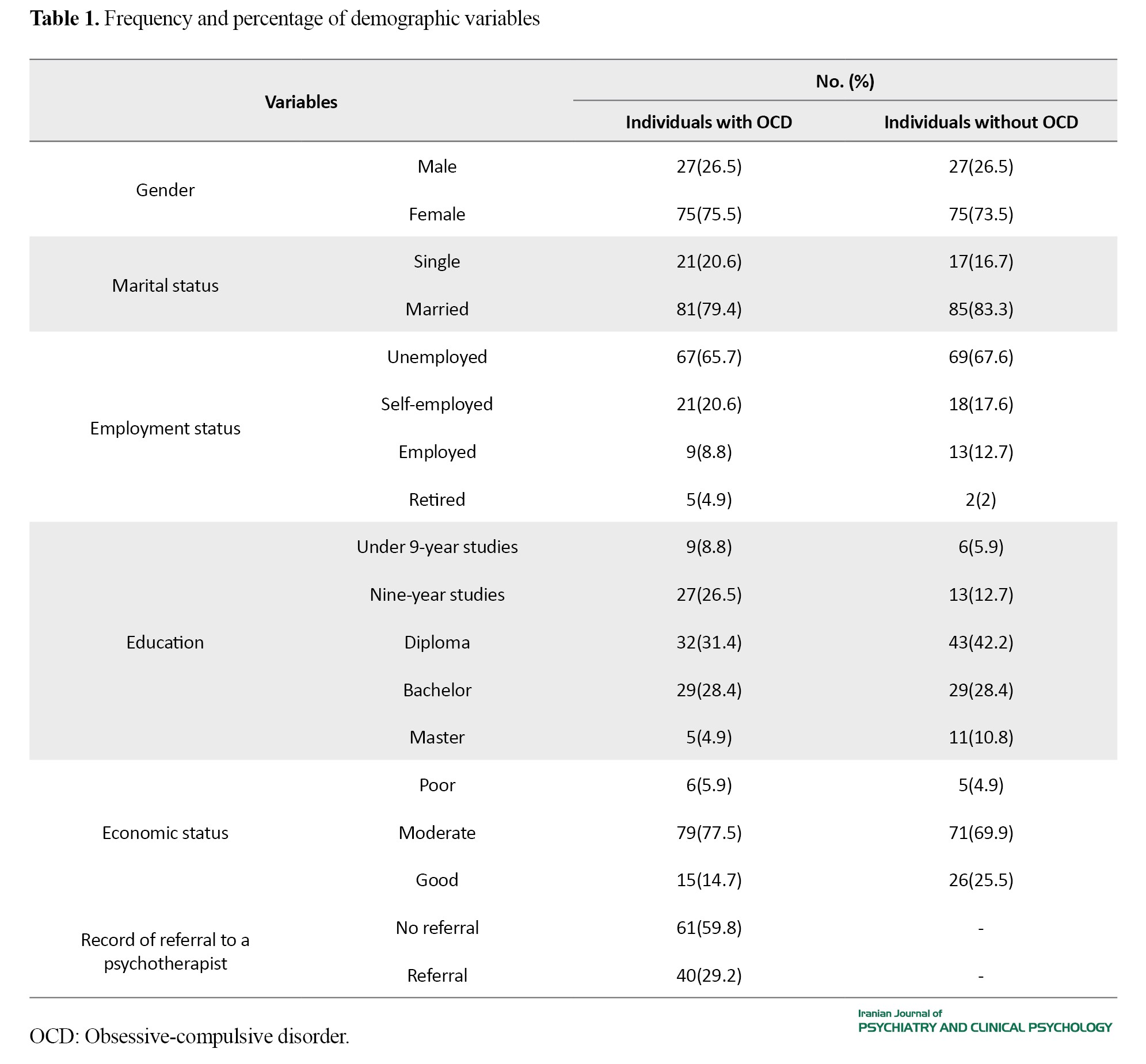
The frequency of demographic variables in the two groups is presented in Table 1.
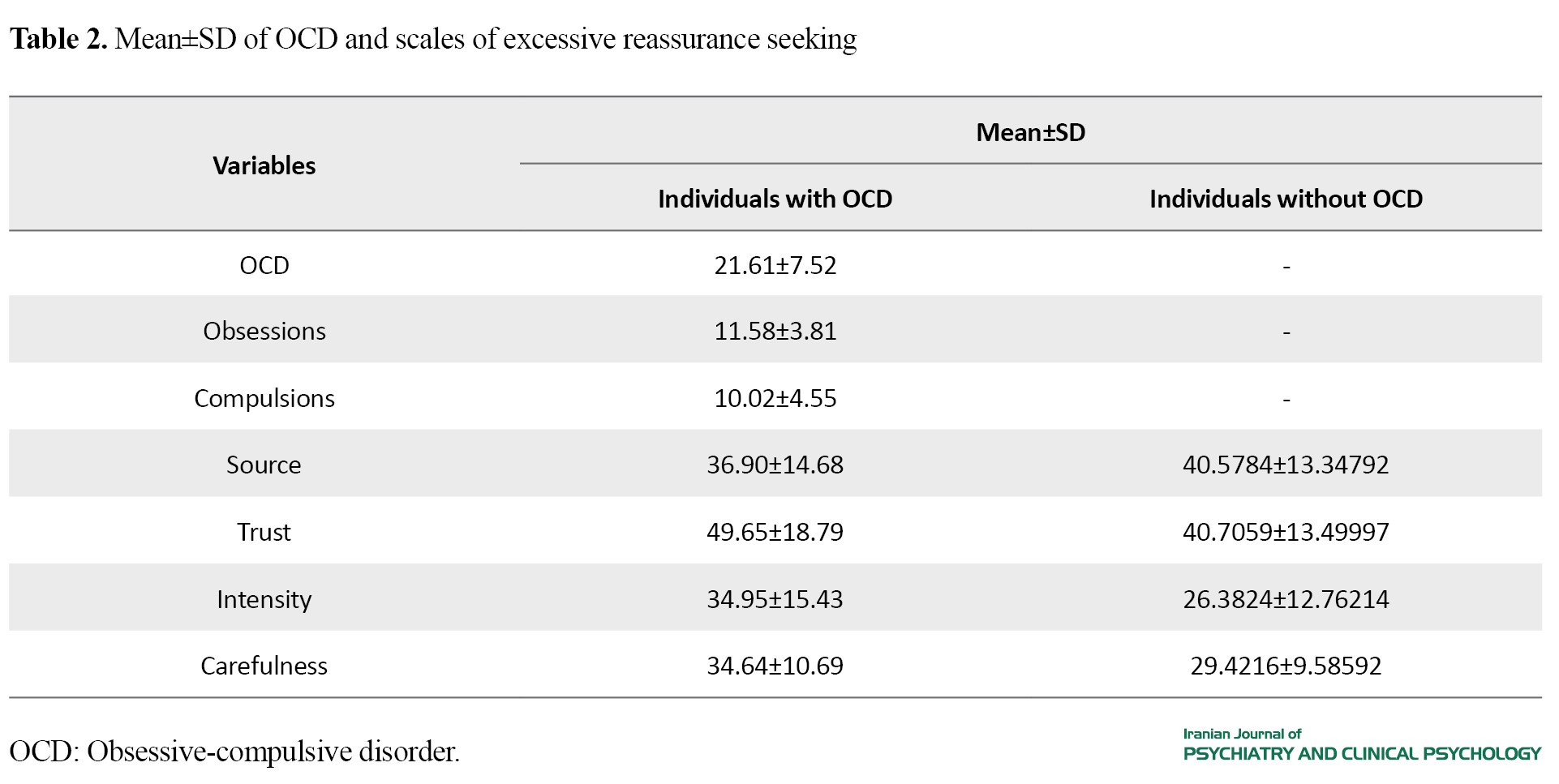
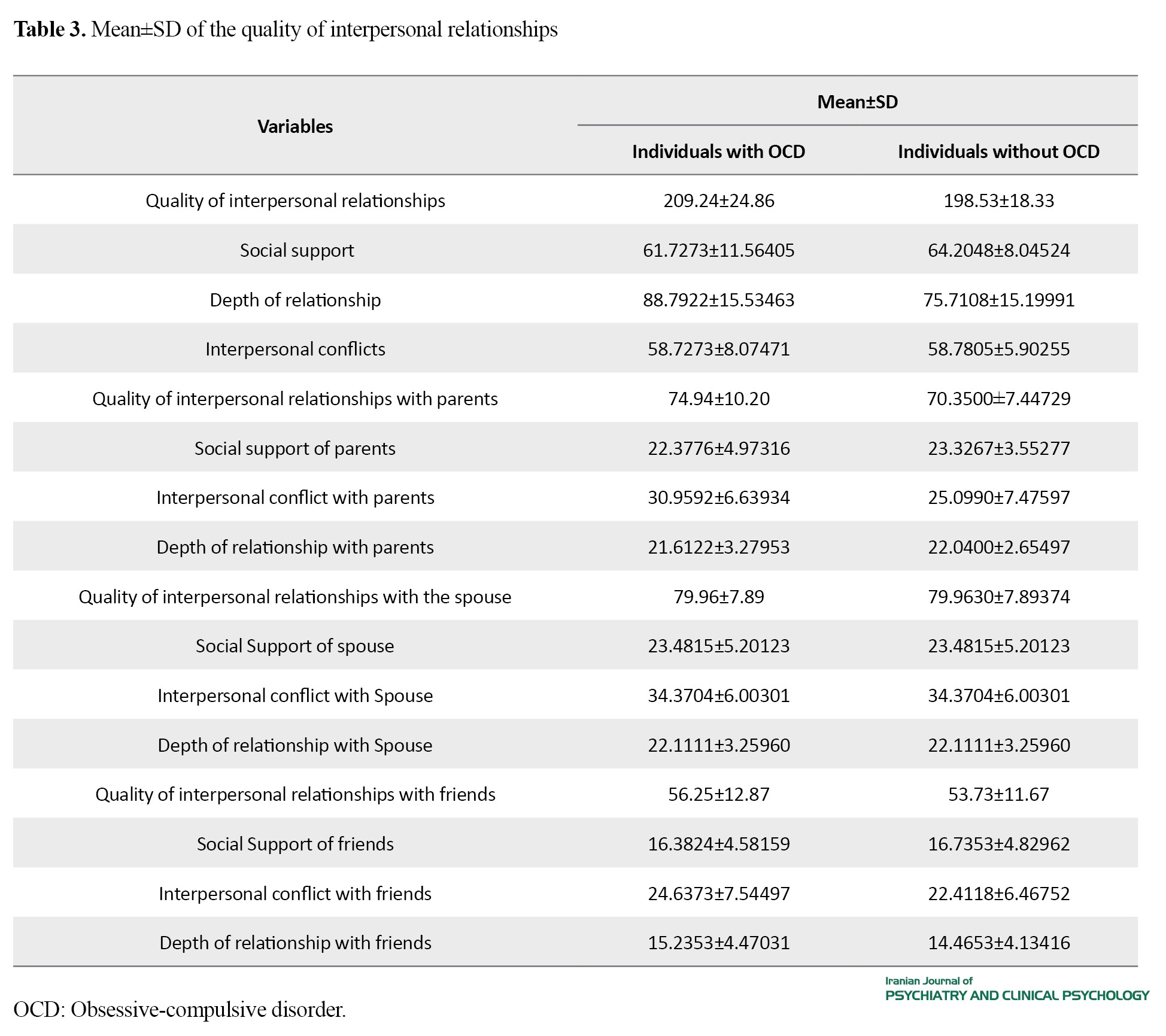
The Mean±SD of the research variables can be seen in Tables 2 and 3.
MANOVA (Table 4) showed that the quality of interpersonal relationships (total score), the quality of interpersonal relationships with parents, and the quality of interpersonal relationships with spouse had significant differences in the two groups.
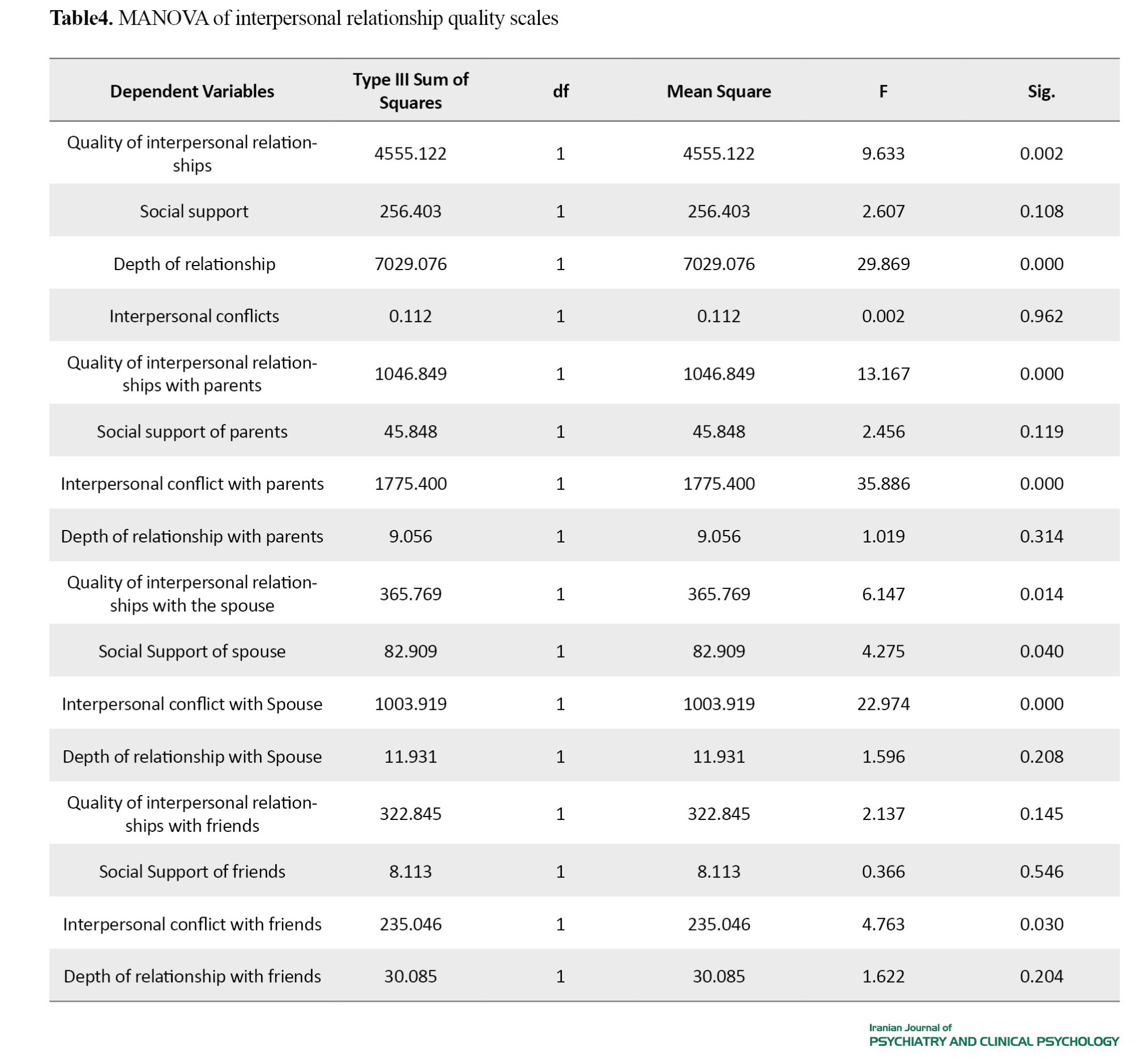
Also, the two groups had significant differences in interpersonal conflict (total score), interpersonal conflict with parents, spouse, and friend, and spouse’s social support. It should be noted that a higher conflict score means less conflict.
Table 5 shows the results of the Pearson correlation test between the quality of interpersonal relationships and the scales of ERS.

According to the findings, there was a significant and positive relationship between the quality of interpersonal relationships and the source (r=0.343), the intensity (r=0.251), and the carefulness of ERS (r=0.285).
Conclusion
The results showed that the quality of interpersonal relationships with spouses and parents is significantly higher in the OCD group than in the healthy group, and the quality of interpersonal relationships has a positive and significant correlation with the source, intensity, and carefulness of ERS. In this regard, the results of this study were in line with those of Halldorsson and Salkovskis [11] and Teleman [17] but were inconsistent with the results reported by Kobori et al. [38].
To account for it, one may refer to the accommodating behavior of families. People suffering from OCD are limited in their communication with others due to the time-consuming nature of obsessions and compulsions, waste of energy, the sensitive nature of some obsessions [37], exhaustion caused by the symptoms of this disorder, and the overlap of OCD with depressive disorders and social anxieties [1].
Because the symptoms of the disorder are more likely to occur at home, the family members of an OCD individual continually accommodate or reassure them. Those individuals find it desirable and supportive, but their family members may be upset and frustrated by the adjustment. In this study, the difference between the OCD and control groups in terms of the mean scores on the quality of interpersonal relationships is justifiable because this variable was evaluated from the perspective of the OCD persons. They may have perceived their interpersonal relationships as good due to family accommodation and companionship, which is not necessarily indicative of the satisfactory quality of interpersonal relationships. Assessing the quality of interpersonal relationships from the perspective of relatives and caregivers of a person with OCD and comparing it with the findings of this study can provide insights and more accurate conclusions. Relationship obsessions, as one of the possible effective variables on the quality of interpersonal relationships in individuals with OCD, were not investigated in this study and can be considered in future research.
Ethical Considerations
Compliance with ethical guidelines
All ethical principles such as the informed consent of the participants, the confidentiality of their information, and their right to leave the research were considered. Ethical approval was obtained from the Research Ethics Committee of Yazd University (Code: IR.YAZD.REC.1400.065).
Funding
This article was extracted from the master’s thesis of Fatemeh Dehghani at the Faculty of Psychology and Educational Sciences, Yazd University. This research did not receive any specific grant from funding agencies in the public, commercial, or not-for profit sectors.
Authors contributions
Conceptualization, Validation, Software, Writing–Original Draft: Maryam Salehzadeh and Fatemeh Dehghani; Data collection: Ghasem Dastjerdi and Fatemeh Dehghani; Formal Analysis: Maryam Salehzadeh, Ali Reza Bakhshayesh, and Fatemeh Dehghani; Investigation: Maryam Salehzadeh, Ghasem Dastjerdi, and Fatemeh Dehghani; Resources, Data Curation: Fatemeh Dehghani; Visualization and Project Administration: Maryam Salehzadeh; Supervision: Maryam Salehzadeh, Ghasem Dastjerdi and, Ali Reza Bakhshayesh; Review & Editing: All authors.
Conflicts of interest
The authors declared no conflict of interest.
Acknowledgments
The authors would like to thank all participants who participated in the study for their cooperation.
References
Obsessive-Compulsive disorder (OCD) is characterized by disturbing, intrusive, anxiety-provoking thoughts (obsessions) and or repetitive behavior (compulsions) [1، 2]. Persistent suspicion or concern about threats or potential harm can prompt people to constantly ask others for information and opinions [3، 7]. This behavior is known as excessive reassurance seeking (ERS) [9]. When reassurance-seeking becomes pervasive in OCD, it can have significant effects on interpersonal relationships [15]. Individuals with OCD often rely on family members and friends. The relatives and caregivers of individuals with OCD are frequently involved in providing reassurance because the families of these individuals are likely to contribute to the symptoms of OCD. This accommodation (ie, assuring) is mostly due to the fact that the symptoms of OCD often and mainly occur at home [17].
Caregivers of individuals with OCD state that persistent reassurance has negative effects on their relations and induces feelings of frustration, anger, and sometimes guilt [16]. In general, the results of previous studies on the interpersonal effects of reassurance-seeking are different and sometimes inconsistent. Halldorsson et al. [16] and Kobori et al. [26] showed that reassurance triggers frustration in caregivers, while Halldorsson and Salkovskis [11] referred to the positive effect of excessive reassurance-seeking (ERS) on interpersonal relationships. Tetelman [17] also reported a positive association between accommodation and relationship satisfaction. In this regard, this research aims to compare the perceived quality of interpersonal relationships in individuals with OCD and a healthy group and investigate the relationship between ERS and the perceived quality of interpersonal relationships in individuals with OCD.
Methods
This study was descriptive and causal-comparative. The statistical population consisted of individuals with OCD who referred to medical centers in Yazd City, Iran, in the fall of 2018 and healthy individuals. In this study, based on the Cochran formula, 102 individuals with OCD and 102 individuals without OCD were selected through purposive sampling. The OCD cases were invited to participate in this study by the psychiatric ward of three medical centers affiliated with Yazd University of Medical Sciences. The inclusion criteria for OCD group were as follows: a) Literacy, b) Absence of other psychiatric disorders based on clinical interviews by a psychiatrist, such as mood disorders, ie, bipolar mood disorder and depression, psychotic disorders, obsessive-compulsive personality disorder and other personality abnormalities, c) Absence of serious medical diseases such as diabetes, Parkinson and neurological diseases like MS, and d) Lack of drug abuse. Trained psychiatrists of Yazd University of Medical Sciences selected the OCD group. Individuals without OCD were chosen in terms of demographic variables corresponding to the OCD group. In addition, the criterion for opting the individuals without OCD to participate in the study was no history of psychiatric diagnosis, clinical complaint, or use of psychiatric drugs. Yale-Brown obsessive-compulsive scale (Y-BOCS) and reassurance seeking questionnaire (ReSQ) (This questionnaire comprises four scales: Source, trust, intensity, and carefulness) were completed by individuals with OCD. Pierce quality of relationship inventory (QRI) (This questionnaire comprises three scales: social support, interpersonal conflicts, and depth of relationship) was completed by both groups, and the data were analyzed using the Pearson correlation and multivariate analysis of variance (MANOVA).
Results
The frequency of demographic variables in the two groups is presented in Table 1.

The Mean±SD of the research variables can be seen in Tables 2 and 3.


MANOVA (Table 4) showed that the quality of interpersonal relationships (total score), the quality of interpersonal relationships with parents, and the quality of interpersonal relationships with spouse had significant differences in the two groups.

Also, the two groups had significant differences in interpersonal conflict (total score), interpersonal conflict with parents, spouse, and friend, and spouse’s social support. It should be noted that a higher conflict score means less conflict.
Table 5 shows the results of the Pearson correlation test between the quality of interpersonal relationships and the scales of ERS.

According to the findings, there was a significant and positive relationship between the quality of interpersonal relationships and the source (r=0.343), the intensity (r=0.251), and the carefulness of ERS (r=0.285).
Conclusion
The results showed that the quality of interpersonal relationships with spouses and parents is significantly higher in the OCD group than in the healthy group, and the quality of interpersonal relationships has a positive and significant correlation with the source, intensity, and carefulness of ERS. In this regard, the results of this study were in line with those of Halldorsson and Salkovskis [11] and Teleman [17] but were inconsistent with the results reported by Kobori et al. [38].
To account for it, one may refer to the accommodating behavior of families. People suffering from OCD are limited in their communication with others due to the time-consuming nature of obsessions and compulsions, waste of energy, the sensitive nature of some obsessions [37], exhaustion caused by the symptoms of this disorder, and the overlap of OCD with depressive disorders and social anxieties [1].
Because the symptoms of the disorder are more likely to occur at home, the family members of an OCD individual continually accommodate or reassure them. Those individuals find it desirable and supportive, but their family members may be upset and frustrated by the adjustment. In this study, the difference between the OCD and control groups in terms of the mean scores on the quality of interpersonal relationships is justifiable because this variable was evaluated from the perspective of the OCD persons. They may have perceived their interpersonal relationships as good due to family accommodation and companionship, which is not necessarily indicative of the satisfactory quality of interpersonal relationships. Assessing the quality of interpersonal relationships from the perspective of relatives and caregivers of a person with OCD and comparing it with the findings of this study can provide insights and more accurate conclusions. Relationship obsessions, as one of the possible effective variables on the quality of interpersonal relationships in individuals with OCD, were not investigated in this study and can be considered in future research.
Ethical Considerations
Compliance with ethical guidelines
All ethical principles such as the informed consent of the participants, the confidentiality of their information, and their right to leave the research were considered. Ethical approval was obtained from the Research Ethics Committee of Yazd University (Code: IR.YAZD.REC.1400.065).
Funding
This article was extracted from the master’s thesis of Fatemeh Dehghani at the Faculty of Psychology and Educational Sciences, Yazd University. This research did not receive any specific grant from funding agencies in the public, commercial, or not-for profit sectors.
Authors contributions
Conceptualization, Validation, Software, Writing–Original Draft: Maryam Salehzadeh and Fatemeh Dehghani; Data collection: Ghasem Dastjerdi and Fatemeh Dehghani; Formal Analysis: Maryam Salehzadeh, Ali Reza Bakhshayesh, and Fatemeh Dehghani; Investigation: Maryam Salehzadeh, Ghasem Dastjerdi, and Fatemeh Dehghani; Resources, Data Curation: Fatemeh Dehghani; Visualization and Project Administration: Maryam Salehzadeh; Supervision: Maryam Salehzadeh, Ghasem Dastjerdi and, Ali Reza Bakhshayesh; Review & Editing: All authors.
Conflicts of interest
The authors declared no conflict of interest.
Acknowledgments
The authors would like to thank all participants who participated in the study for their cooperation.
References
- American Psychiatric Association. Diagnostic and statistical manual of mental disorders: DSM-5. Washington: American Psychiatric Association; 2013. [DOI:10.1176/appi.books.9780890425596]
- Rachman S, Hodgson RJ. Obsessions and compulsions. Upper Saddle River: Prentice-Hall; 1980. [Link]
- Radomsky AS, Alcolado GM, Abramowitz JS, Alonso P, Belloch A, Bouvard M, et al. Part 1-You can run but you can’t hide: Intrusive thoughts on six continents. Journal of Obsessive-Compulsive and Related Disorders. 2014; 3(3):269-79. [DOI:10.1016/j.jocrd.2013.09.002]
- World Health Organization (WHO). The global burden of disease. Geneva: World Health Organization; 2004. [Link]
- Toffolo MBJ. Better super safe than slightly sorry?: Reciprocal relationships between checking behavior and cognitive symptoms in obsessive-compulsive disorder [doctoral dissertation]. Utrecht: Utrecht University; 2015. [Link]
- Rachman S. A cognitive theory of compulsive checking. Behaviour Research and Therapy. 2002; 40(6):625-39. [DOI:10.1016/S0005-7967(01)00028-6] [PMID]
- Parrish CL, Radomsky AS. Why do people seek reassurance and check repeatedly? An investigation of factors involved in compulsive behavior in OCD and depression. Journal of Anxiety Disorders. 2010; 24(2):211-22. [DOI:10.1016/j.janxdis.2009.10.010] [PMID]
- Radomsky AS, Dugas MJ, Alcolado GM, Lavoie SL. When more is less: Doubt, repetition, memory, metamemory, and compulsive checking in OCD. Behaviour Research and Therapy. 2014; 59:30-9. [DOI:10.1016/j.brat.2014.05.008] [PMID]
- Leonhart MW, Radomsky AS. Responsibility causes reassurance seeking, too: An experimental investigation. Journal of Obsessive-Compulsive and Related Disorders. 2019; 20:66-74. [DOI:10.1016/j.jocrd.2017.10.005]
- Halldorsson B. “ Please help me”: Excessive reassurance seeking as an interpersonal process in obsessive compulsive disorder and health anxiety [doctoral dissertation]. Bath: University of Bath; 2015. [Link]
- Halldorsson B, Salkovskis PM. Why do people with OCD and health anxiety seek reassurance excessively? An investigation of differences and similarities in function. Cognitive Therapy and Research. 2017; 41(4):619-31. [DOI:10.1007/s10608-016-9826-5] [PMID]
- Abramowitz JS, Schwartz SA, Whiteside SP. A contemporary conceptual model of hypochondriasis. Mayo Clinic Proceedings. 2002; 77(12):1323-30. [DOI:10.4065/77.12.1323] [PMID]
- Salkovskis PM, Warwick HM. Morbid preoccupations, health anxiety and reassurance: A cognitive-behavioural approach to hypochondriasis. Behaviour Research and Therapy. 1986; 24(5):597-602. [DOI:10.1016/0005-7967(86)90041-0] [PMID]
- Salkovskis PM. Obsessional-compulsive problems: A cognitive-behavioural analysis. Behaviour Research and Therapy. 1985; 23(5):571-83. [DOI:10.1016/0005-7967(85)90105-6] [PMID]
- Neal R. What Are You Looking For? Psychometric and experimental investigations of reassurance seeking in obsessive-compulsive disorder [doctoral dissertation]. Montreal: Concordia University; 2019. [Link]
- Halldorsson B, Salkovskis PM, Kobori O, Pagdin R. I do not know what else to do: Caregivers’ perspective on reassurance seeking in OCD. Journal of Obsessive-Compulsive and Related Disorders. 2016; 8:21-30. [DOI:10.1016/j.jocrd.2015.11.003]
- Tetelman A. The Relationship between Obsessive-Compulsive Disorder, Partner Accommodation, Adult Attachment Styles, and Relationship Satisfaction [doctoral dissertation]. San Diego: Alliant International University; 2018. [Link]
- Whisman MA, Baucom DH. Intimate relationships and psychopathology. Clinical Child and Family Psychology Review. 2012; 15(1):4-13. doi [DOI:10.1007/s10567-011-0107-2] [PMID]
- Albert U, Bogetto F, Maina G, Saracco P, Brunatto C, Mataix-Cols D. Family accommodation in obsessive-compulsive disorder: Relation to symptom dimensions, clinical and family characteristics. Psychiatry Research. 2010; 179(2):204-11. [DOI:10.1016/j.psychres.2009.06.008] [PMID]
- Boeding SE, Paprocki CM, Baucom DH, Abramowitz JS, Wheaton MG, Fabricant LE, et al. Let me check that for you: Symptom accommodation in romantic partners of adults with obsessive-compulsive disorder. Behaviour Research and Therapy. 2013; 51(6):316-22. [DOI:10.1016/j.brat.2013.03.002] [PMID]
- Salkovskis PM. Avoidance behaviour is motivated by threat beliefs: A possible resolution of the cognition-behaviour debate. Trends in Cognitive and Behavioural Therapies. 1996; 25-42. [Link]
- Torres AR, Hoff NT, Padovani CR, Ramos-Cerqueira ATdA. Dimensional analysis of burden in family caregivers of patients with obsessive-compulsive disorder. Psychiatry and Clinical Neurosciences. 2012; 66(5):432-41. [DOI:10.1111/j.1440-1819.2012.02365.x] [PMID]
- Holahan CJ, Moos RH, Bonin LA. Social context and depression: An integrative stress and coping framework. In: Joiner T, Coyne JC, editors. The interactional nature of depression: Advances in interpersonal approaches. New York: American Psychological Association; 1999. [Link]
- Amir N, Freshman M, Foa EB. Family distress and involvement in relatives of obsessive-compulsive disorder patients. Journal of Anxiety Disorders. 2000; 14(3):209-17. [DOI:10.1016/S0887-6185(99)00032-8] [PMID]
- Abbey RD, Clopton JR, Humphreys JD. Obsessive-compulsive disorder and romantic functioning. Journal of Clinical Psychology. 2007; 63(12):1181-92. [DOI:10.1002/jclp.20423] [PMID]
- Kobori O, Salkovskis PM, Pagdin R, Read J, Halldorsson B. Carer’s perception of and reaction to reassurance seeking in obsessive compulsive disorder. The Cognitive Behaviour Therapist. 2017; 10:e7. [DOI:10.1017/S1754470X17000095]
- Goodman WK, Price LH, Rasmussen SA, Mazure C, Delgado P, Heninger GR, et al. The yale-brown obsessive compulsive scale: II. Validity. Archives of General Psychiatry. 1989; 46(11):1012-6. [DOI:10.1001/archpsyc.1989.01810110054008] [PMID]
- Deacon BJ, Abramowitz JS. The Yale-Brown Obsessive Compulsive Scale: Factor analysis, construct validity, and suggestions for refinement. Journal of Anxiety Disorders. 2005; 19(5):573-85. [DOI:10.1016/j.janxdis.2004.04.009] [PMID]
- Baer L, Brown-Beasley MW, Sorce J, Henriques AI. Computer-assisted telephone administration of a structured interview for obsessive-compulsive disorder. The American Journal of Psychiatry. 1993; 150(11):1737-8. [DOI:10.1176/ajp.150.11.1737] [PMID]
- Steketee G, Frost R, Bogart K. The Yale-Brown obsessive compulsive scale: Interview versus self-report. Behaviour Research and Therapy. 1996; 34(8):675-84. [DOI:10.1016/0005-7967(96)00036-8] [PMID]
- Rajezi Esfahani S, Motaghipour Y, Kamkari K, Zahiredin A, Janbozorgi M. Reliability and validity of the persian version of the yale-brown obsessive-compulsive scale (Y-BOCS). Iranian Journal of Psychiatry and Clinical Psychology. 2012; 17(4):297–303. [Link]
- Kobori O, Salkovskis PM. Patterns of reassurance seeking and reassurance-related behaviours in OCD and anxiety disorders. Behavioural and Cognitive Psychotherapy. 2013; 41(1):1-23. [DOI:10.1017/S1352465812000665] [PMID]
- Kobori O, Sawamiya Y, Iyo M, Shimizu E. A comparison of manifestations and impact of reassurance seeking among Japanese individuals with OCD and depression. Behavioural and Cognitive Psychotherapy. 2015; 43(5):623-34. [DOI:10.1017/S1352465814000277] [PMID]
- Kobori O, Sawamiya Y. Development of the Japanese version of Reassurance Seeking. Questionnaire. 2012. [Unpublished].
- Pierce GR, Sarason IG, Sarason BR. General and relationship-based perceptions of social support: Are two constructs better than one? Journal of personality and Social Psychology. 1991; 61(6):1028. [DOI:10.1037/0022-3514.61.6.1028] [PMID]
- Hosseini Ghadamgahi J, Dojakam M, Bayanzadeh SA, Feiz A. [Quality of social relationships, stress levels and coping strategies in cardiovascular patients (Persian)]. Iranian Journal of Psychiatry and Clinical Psychology. 1998; 4(1):14-24. [Link]
- Black DW, Gaffney G, Schlosser S, Gabel J. The impact of obsessive-compulsive disorder on the family: Preliminary findings. The Journal of Nervous and Mental Disease. 1998; 186(7):440-2. [DOI:10.1097/00005053-199807000-00010] [PMID]
- Kobori O, Salkovskis PM, Read J, Lounes N, Wong V. A qualitative study of the investigation of reassurance seeking in obsessive-compulsive disorder. Journal of Obsessive-Compulsive and Related Disorders. 2012; 1(1):25-32. [DOI:10.1016/j.jocrd.2011.09.001]
- Calvocoressi L, Mazure CM, Kasl SV, Skolnick J, Fisk D, Vegso SJ, et al. Family accommodation of obsessive-compulsive symptoms: Instrument development and assessment of family behavior. The Journal of Nervous and Mental Disease. 1999; 187(10):636-42. [DOI:10.1097/00005053-199910000-00008] [PMID]
- Lee EB, Rufino KA, Cuenod MM, Zhang CC, Gong H, Zhang Y, et al. Family accommodation in Chinese individuals with obsessive-compulsive disorder. PsyCh Journal. 2021; 10(2):295-304. [DOI:10.1002/pchj.425] [PMID]
- Abramowitz JS, Baucom DH, Boeding S, Wheaton MG, Pukay-Martin ND, Fabricant LE, et al. Treating obsessive-compulsive disorder in intimate relationships: A pilot study of couple-based cognitive-behavior therapy. Behavior Therapy. 2013; 44(3):395-407. [DOI:10.1016/j.beth.2013.02.005] [PMID]
- Abramowitz JS. An interpersonal perspective on the conceptualization and treatment of OCD. In: Abramowitz JS, McKay D, Storch EO, editors. The wiley handbook of obsessive compulsive disorders. Hoboken: Wiley; 2017. [DOI:10.1002/9781118890233.ch35]
- Yazdi-Ravandi S, Matinnia N, Shamsaei F, Ahmadpanah M, Shams J, Ghaleiha A. Experiences of interpersonal relationships in patients with obsessive-compulsive disorder: A qualitative study in Iran. Pertanika Journal of Social Sciences & Humanities. 2018; 26(3): 1673-83. [Link]
Type of Study: Original Research |
Subject:
Psychiatry and Psychology
Received: 2024/09/6 | Accepted: 2025/04/8 | Published: 2025/08/1
Received: 2024/09/6 | Accepted: 2025/04/8 | Published: 2025/08/1
| Rights and permissions | |
 |
This work is licensed under a Creative Commons Attribution-NonCommercial 4.0 International License. |






