Fri, Jul 11, 2025
| فارسی
Volume 23, Issue 3 (Fall 2017)
IJPCP 2017, 23(3): 306-319 |
Back to browse issues page
Download citation:
BibTeX | RIS | EndNote | Medlars | ProCite | Reference Manager | RefWorks
Send citation to:



BibTeX | RIS | EndNote | Medlars | ProCite | Reference Manager | RefWorks
Send citation to:
Shahrivar Z, Mahmoodi Gharaei J, Zare'i M, Zarrabi M, Shirazi E. Clinical Characteristics, Function, Quality of Life, and Premorbid Adjustment in Children and Adolescents With First-Episode Psychosis Admitted at Roozbeh Hospital. IJPCP 2017; 23 (3) :306-319
URL: http://ijpcp.iums.ac.ir/article-1-2490-en.html
URL: http://ijpcp.iums.ac.ir/article-1-2490-en.html
1- Research Center for Cognitive and Behavioral Sciences, Roozbeh Hospital, Tehran University of Medical Sciences, Tehran, Iran-Department of Psychiatry, School of Medicine, Tehran University of Medical Sciences, Tehran, Iran , E-mail: sharivar@sina.tums.ac.ir
2- Research Center for Cognitive and Behavioral Sciences, Roozbeh Hospital, Tehran University of Medical Sciences, Tehran, Iran.
3- Department of Psychiatry, Roozbeh Hospital, Tehran University of Medical Sciences, Tehran, Iran
4- Roozbeh Hospital, Tehran University of Medical Sciences, Tehran, Iran
5- Mental Health Research Center, School of Behavioral Sciences and Mental Health (Tehran Institute of Psychiatry), Iran University of Medical Sciences, Tehran, Iran
2- Research Center for Cognitive and Behavioral Sciences, Roozbeh Hospital, Tehran University of Medical Sciences, Tehran, Iran.
3- Department of Psychiatry, Roozbeh Hospital, Tehran University of Medical Sciences, Tehran, Iran
4- Roozbeh Hospital, Tehran University of Medical Sciences, Tehran, Iran
5- Mental Health Research Center, School of Behavioral Sciences and Mental Health (Tehran Institute of Psychiatry), Iran University of Medical Sciences, Tehran, Iran
Full-Text [PDF 6601 kb]
(2753 Downloads)
| Abstract (HTML) (7877 Views)
Full-Text: (5487 Views)
Extended Abstract
1. Introduction
First Episode Psychosis (FEP) refers to the emergence of psychotic symptoms such as delusion, hallucination, disorganized behavior, and abnormal effects before the age of 18 years. Early diagnosis and treatment of FEP have been considered as an important field of research in the past two decades, confirming the effect of early preventive strategies. Research on adults with FEP has been conducted in Iran evaluating diagnostic stability, course, and clinical consequences [5-7]; however, the different aspects of FEP in children and adolescents in Iran have seldom been evaluated. Therefore, this study was done to evaluate the demographic and clinical characteristics of inpatient children and adolescents with FEP at a tertiary psychiatric hospital.
2. Method
During a two-year prospective study (2013-2014), all consecutive admissions in the child and adolescent psychiatric ward were evaluated in terms of FEP. Among them, those whose symptoms were substance-induced or had medical etiology were excluded. The study aims and process were explained to the participants, and their parents and oral assent and consent were received from them. Diagnoses were made using clinical assessment by a child and adolescent psychiatrist and confirmed by a semi-structured interview using the Kiddie Schedule for Affective Disorder and Schizophrenia-Present and lifetime Version-Persian Version.
The Positive and Negative Symptoms Scale (PANSS) was used by a clinician to rate the psychotic features of FEP in the participants. Moreover, to assess the participants’ adaptation before the emergence of psychosis, the Premorbid Adjustment Scale (PAS) was accomplished for interviewing the participants and their parents. The study clinician completed the Clinical Global Assessment Scale (CGAS) to rate the level of general functioning in the participants. The World Health Organization Quality of Life- brief questionnaire (WHOQOL-Bref) was completed by the participants to determine the quality of life variables. The participants were receiving treatment as per the usual protocol in the hospital. To analyze the data, the descriptive method was used to assess the prevalence and means. The Spearman’s correlation analysis was performed to test the association between the variables.
3. Results
A total of 44 participants (47.7% boys) with FEP were enrolled in the study. Their mean age was 193.11(21.5) months, and 70.5% were students. Among them, 43.2% lived in the capital and the others were referred from other states of the country. The history of psychiatric disorders was positive in 18.2% of first- and second-degree relatives of the participants. Before admission, half of the participants had visited psychiatrists, and nearly 40% had been referred to psychologists. The duration of untreated psychosis was more than 6 months in 13% of the participants while 31.2% of the youth were admitted in the first 2 weeks. In terms of psychiatric diagnoses, 68.3% were suffering from Bipolar Disorder (BD) and 15.9% from Schizophrenia. Brief psychotic disorder and psychosis not otherwise specialized were found in 4.5% and 2.3% patients, respectively.
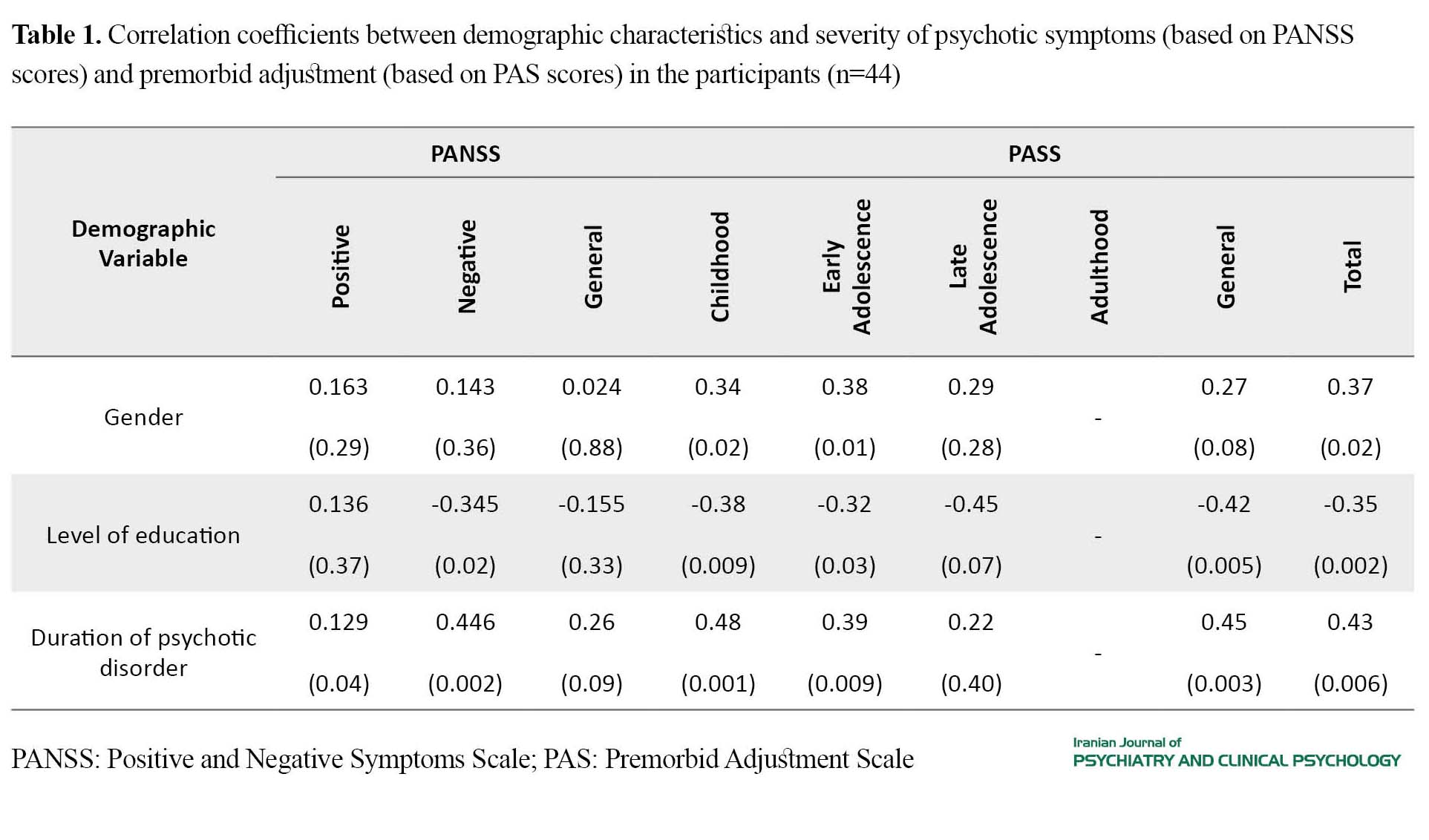
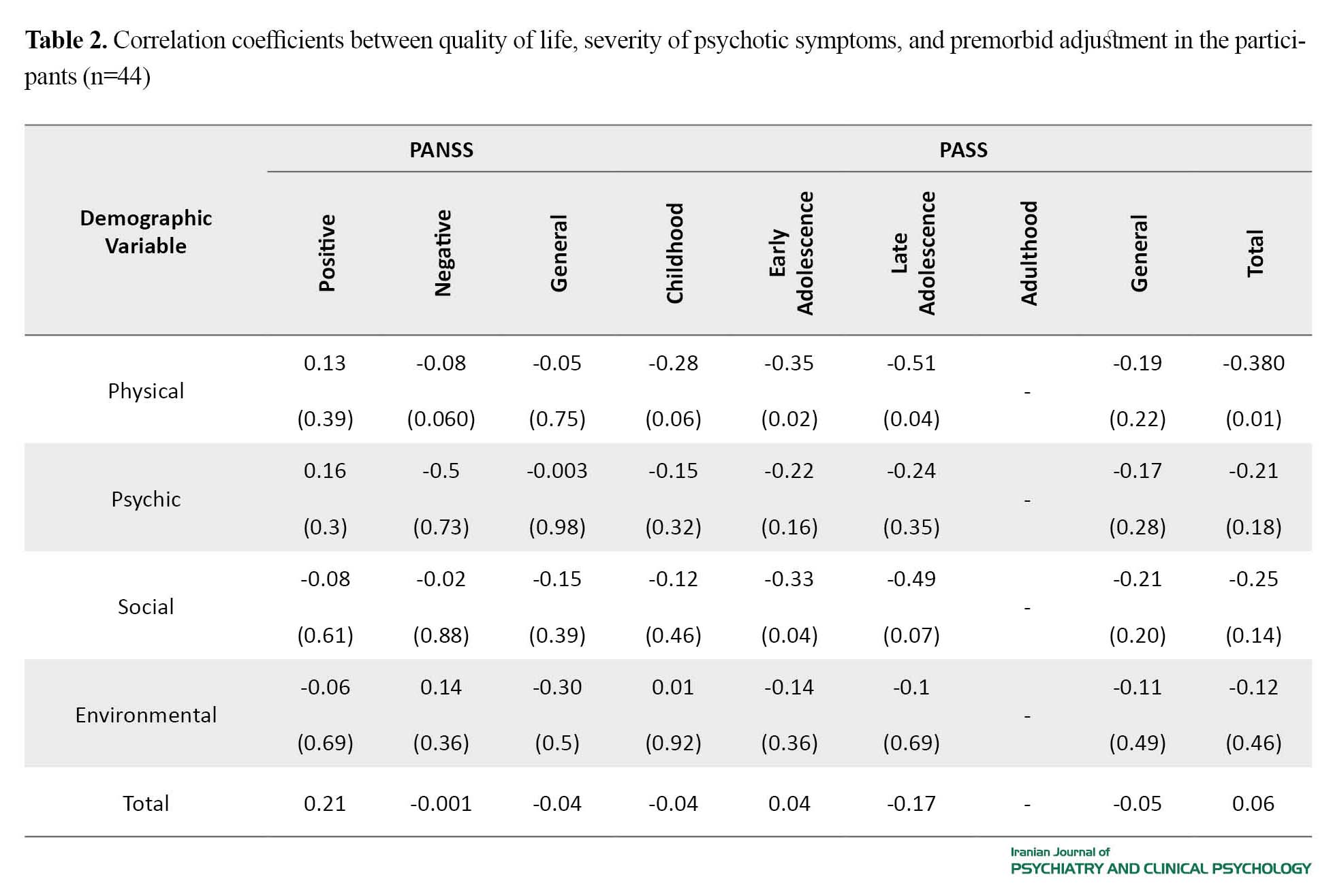
The most prevalent comorbid disorders were obsessive-compulsive disorder (11.3%), attention-deficit hyperactivity disorder (9%), specific phobia (6.8%), and autism (4.5%). Intellectual disability was found in 11.4%, and medical disease in one-third of the participants. More than 40% of the participants had problems approaching with mental health services. Poor adjustment before the emergence of psychosis was negatively related with academic level and positively consistent with female gender, suicidal risk, and duration of psychotic disorder (P<0.05). The level of premorbid global functioning was lower than 80% in 93% of the participants. This score was less than 40% in 95% of them during admission. Correlation coefficients between demographic characteristics and severity of psychotic symptoms (based on PANSS scores) and premorbid adjustment (based on PAS scores) in the participants (n=44)are shown in Table 1. Table 2 demonstrates correlation coefficients between quality of life, severity of psychotic symptoms, and premorbid adjustment in the participants. 4. Conclusion
This study used limited prospective cohorts of children/adolescents who experienced symptoms of an episode of psychosis for the first time. Among this group of inpatients in a psychiatric hospital, bipolar disorder was the most common diagnosis and non-affective psychotic disorders came second. This fact was in line with some previous findings while it was inconsistent with the studies that showed Schizophrenia and Schizophreniform disorders as the most common diagnoses in children and adolescents with FEP [1-4]. These different findings can be interpreted by various methods of assessment and case findings; for example, outpatient versus inpatient enrollment.
The participants in our study suffered from severe psychiatric symptoms and risk of suicide. Appropriate mental health services were not available for many of these children and adolescents, and they were at risk of chronicity of psychosis and its lifelong negative consequences. FEP was consistent with poor premorbid adjustment and severe global functioning impairment. These findings confirm the need for early prevention for vulnerable individuals, as well as appropriate pharmacologic and non-pharmacologic interventions.
Acknowledgments
This paper was financially supported by Tehran University of Medical Sciences (Grant Number: 10294).
Conflict of Interest
The authors declare no conflicts of interest.
1. Introduction
First Episode Psychosis (FEP) refers to the emergence of psychotic symptoms such as delusion, hallucination, disorganized behavior, and abnormal effects before the age of 18 years. Early diagnosis and treatment of FEP have been considered as an important field of research in the past two decades, confirming the effect of early preventive strategies. Research on adults with FEP has been conducted in Iran evaluating diagnostic stability, course, and clinical consequences [5-7]; however, the different aspects of FEP in children and adolescents in Iran have seldom been evaluated. Therefore, this study was done to evaluate the demographic and clinical characteristics of inpatient children and adolescents with FEP at a tertiary psychiatric hospital.
2. Method
During a two-year prospective study (2013-2014), all consecutive admissions in the child and adolescent psychiatric ward were evaluated in terms of FEP. Among them, those whose symptoms were substance-induced or had medical etiology were excluded. The study aims and process were explained to the participants, and their parents and oral assent and consent were received from them. Diagnoses were made using clinical assessment by a child and adolescent psychiatrist and confirmed by a semi-structured interview using the Kiddie Schedule for Affective Disorder and Schizophrenia-Present and lifetime Version-Persian Version.
The Positive and Negative Symptoms Scale (PANSS) was used by a clinician to rate the psychotic features of FEP in the participants. Moreover, to assess the participants’ adaptation before the emergence of psychosis, the Premorbid Adjustment Scale (PAS) was accomplished for interviewing the participants and their parents. The study clinician completed the Clinical Global Assessment Scale (CGAS) to rate the level of general functioning in the participants. The World Health Organization Quality of Life- brief questionnaire (WHOQOL-Bref) was completed by the participants to determine the quality of life variables. The participants were receiving treatment as per the usual protocol in the hospital. To analyze the data, the descriptive method was used to assess the prevalence and means. The Spearman’s correlation analysis was performed to test the association between the variables.
3. Results
A total of 44 participants (47.7% boys) with FEP were enrolled in the study. Their mean age was 193.11(21.5) months, and 70.5% were students. Among them, 43.2% lived in the capital and the others were referred from other states of the country. The history of psychiatric disorders was positive in 18.2% of first- and second-degree relatives of the participants. Before admission, half of the participants had visited psychiatrists, and nearly 40% had been referred to psychologists. The duration of untreated psychosis was more than 6 months in 13% of the participants while 31.2% of the youth were admitted in the first 2 weeks. In terms of psychiatric diagnoses, 68.3% were suffering from Bipolar Disorder (BD) and 15.9% from Schizophrenia. Brief psychotic disorder and psychosis not otherwise specialized were found in 4.5% and 2.3% patients, respectively.
The most prevalent comorbid disorders were obsessive-compulsive disorder (11.3%), attention-deficit hyperactivity disorder (9%), specific phobia (6.8%), and autism (4.5%). Intellectual disability was found in 11.4%, and medical disease in one-third of the participants. More than 40% of the participants had problems approaching with mental health services. Poor adjustment before the emergence of psychosis was negatively related with academic level and positively consistent with female gender, suicidal risk, and duration of psychotic disorder (P<0.05). The level of premorbid global functioning was lower than 80% in 93% of the participants. This score was less than 40% in 95% of them during admission. Correlation coefficients between demographic characteristics and severity of psychotic symptoms (based on PANSS scores) and premorbid adjustment (based on PAS scores) in the participants (n=44)are shown in Table 1. Table 2 demonstrates correlation coefficients between quality of life, severity of psychotic symptoms, and premorbid adjustment in the participants. 4. Conclusion
This study used limited prospective cohorts of children/adolescents who experienced symptoms of an episode of psychosis for the first time. Among this group of inpatients in a psychiatric hospital, bipolar disorder was the most common diagnosis and non-affective psychotic disorders came second. This fact was in line with some previous findings while it was inconsistent with the studies that showed Schizophrenia and Schizophreniform disorders as the most common diagnoses in children and adolescents with FEP [1-4]. These different findings can be interpreted by various methods of assessment and case findings; for example, outpatient versus inpatient enrollment.
The participants in our study suffered from severe psychiatric symptoms and risk of suicide. Appropriate mental health services were not available for many of these children and adolescents, and they were at risk of chronicity of psychosis and its lifelong negative consequences. FEP was consistent with poor premorbid adjustment and severe global functioning impairment. These findings confirm the need for early prevention for vulnerable individuals, as well as appropriate pharmacologic and non-pharmacologic interventions.
Acknowledgments
This paper was financially supported by Tehran University of Medical Sciences (Grant Number: 10294).
Conflict of Interest
The authors declare no conflicts of interest.
References
- Schimmelmann BG, Conus P, Schacht M, Mcgorry P, Lambert M. Predictors of service disengagement in first admitted adolescents with psychosis. Journal of the American Academy of Child & Adolescent Psychiatry. 2006; 45(8):990–9. doi: 10.1097/01.chi.0000223015.29530.65
- Noguera A, Ballesta P, Baeza I, Arango C, de la Serna E, González Pinto A, et al. Twenty four months of antipsychotic treatment in children and adolescents with first psychotic episode. Journal of Clinical Psychopharmacology. 2013; 33(4):463–71. doi: 10.1097/jcp.0b013e3182962480
- Castro Fornieles J, Parellada M, Gonzalez Pinto A, Moreno D, Graell M, Baeza I, et al. The child and adolescent first-episode psychosis study (CAFEPS): Design and baseline results. Schizophrenia Research. 2007; 91(1-3):226–37. doi: 10.1016/j.schres.2006.12.004
- Janssen J, Reig S, Parellada M, Moreno D, Graell M, Fraguas D, et al. Regional gray matter volume deficits in adolescents with first-episode psychosis. Journal of the American Academy of Child & Adolescent Psychiatry. 2008; 47(11):1311–20. doi: 10.1097/chi.0b013e318184ff48
- Amini H, Alaghbandrad J, Omid A, Sharifi V, Davari Ashtiani R, Momeni F, et al. Diagnostic stability in patients with first-episode psychosis. Australasian Psychiatry. 2005; 13(4):388–92. doi: 10.1111/j.1440-1665.2005.02199.x
- Alaghbandrad J., Amini H., Sharifi V., Dashti B. A 2 year followup study on patients with first episode psychosis admitted to Roozbeh Hospital: Demographic and clinical characteristics and comparison of a specialized program and treatment as usual, Final Report. Tehran: Tehran University of Medical Sciences; 2010.
- Sharifi V, Amini H, Shahrivar Z, Mottaghipour Y, Mahmoudi Gharaee J, Alaghband Rad J. Courseof psychotic disorders: A 3-year follow up study of patients with first episode psychosis. Iranian Journal of Psychiatry and Clinical Psychology. 2014; 20(1):35-42.
- Shahrivar Z, Alaghband Rad J, Mahmoudi Gharaie J, Seddigh A, Salesian N, Jalali Roodsari M, et al. The efficacy of an integrated treatment in comparison with treatment as usual in a group of children and adolescents with first episode psychosis during a two year follow up. Iranian Journal of Psychiatry and Clinical Psychology. 2012; 18(2):115-37.
- Kaufman J, Birmaher B, Brent D, Rao U, Flynn C, Moreci P, et al. Schedule for affective disorders and schizophrenia for school age children-present and lifetime version (K-SADS-PL): Initial reliability and validity data. Journal of the American Academy of Child & Adolescent Psychiatry. 1997; 36(7):980–8. doi: 10.1097/00004583-199707000-00021
- Shahrivar Z, Kousha M, Moallemi S, Tehrani Doost M, Alaghband Rad J. The reliability and validity of kiddie schedule for affective disorders and schizophrenia present and life time version - persian version. Child and Adolescent Mental Health. 2010; 15(2):97–102. doi: 10.1111/j.1475-3588.2008.00518.x
- Kay SR, Fiszbein A, Opler LA. The positive and negative syndrome scale (PANSS) for schizophrenia. Schizophrenia Bulletin. 1987; 13(2):261–76. doi: 10.1093/schbul/13.2.261
- Bates MP. The child and adolescent functional assessment scale (CAFAS): Review and current status. Clinical Child and Family Psychology Review. 2001; 4(1):63-84.
- Patterson DA, Lee MS. Field trial of the Global Assessment of Functioning Scale--Modified. American Journal of Psychiatry. 1995; 152(9):1386–8. doi: 10.1176/ajp.152.9.1386
- Shaffer D, Gould MS, Brasic J, Ambrosini P, Fisher P, Bird H, et al. A children's global assessment scale (CGAS). Archives of General psychiatry. 1983; 40(11):1228-31. doi: 10.1001/archpsyc.1983.01790100074010
- Blake K, Cangelosi S, Johnson Brooks S, Belcher HME. Reliability of the GAF and CGAS with children exposed to trauma. Child Abuse & Neglect. 2007; 31(8):909–15. doi: 10.1016/j.chiabu.2006.12.017
- World Health Organization. WHOQOL-BREF: Introduction, administration and scoring, Field Trial version. Geneva: World Health Organization; 1996.
- Nedjat S, Montazeri A, Holakouie K, Mohammad K, Majdzadeh R. Psychometric properties of the Iranian interview-administered version of the World Health Organization's Quality of Life Questionnaire (WHOQOL-BREF): A population based study. BMC Health Services Research. 2008; 8(1):61. doi: 10.1186/1472-6963-8-61
- Nejat SA, Montazeri A, Holakouie Naieni K, Mohammad KA, Majdzadeh SR. The World Health Organization quality of Life (WHOQOL-BREF) questionnaire: Translation and validation study of the Iranian version. Journal of School of Public Health and Institute of Public Health Research. 2006; 4(4):1-2.
- Krauss H, Marwinski K, Held T, Rietschel M, Freyberger HJ. Reliability and validity of the Premorbid Adjustment Scale (PAS) in a German sample of schizophrenic and schizoaffective patients. European Archives of Psychiatry and Clinical Neuroscience. 1998; 248(6):277–81. doi: 10.1007/s004060050050
- Brill N, Reichenberg A, Weiser M, Rabinowitz J. Validity of the premorbid adjustment scale. Schizophrenia Bulletin. 2008; 34(5):981–3. doi: 10.1093/schbul/sbm128
- Mahmoodi Gharaei J, Basirnia A, Abedi N, Shadloo B, Jafari S, Salesian N, et al. Association of premorbid adjustment with symptom profile and quality of life in first episode psychosis in a tertiary hospital in Tehran, Iran. Iranian Journal of P sychiatry. 2010; 5(1):23-27. PMCID: PMC3430406
- Harper A, Power M, Orley J, Herrman H, Schofield H, Murphy B, et al. Development of the World Health Organization WHOQOL-BREF Quality of Life Assessment. Psychological Medicine. 1998; 28(3):551–8. doi: 10.1017/s0033291798006667
- Driver DI, Gogtay N, Rapoport JL. Childhood onset schizophrenia and early onset schizophrenia spectrum disorders. Child and Adolescent Psychiatric Clinics of North America. 2013; 22(4):539–55. doi: 10.1016/j.chc.2013.04.001
- Schreier HA. Hallucinations in nonpsychotic children: More Common than we think. Journal of the American Academy of Child & Adolescent Psychiatry. 1999; 38(5):623–5. doi: 10.1097/00004583-199905000-00028
- Jarbin H., Ott Y., Von Knorring AL. Adult outcome of social function in adolescent onset schizophrenia and affective psychosis. Journal of the American Academy of Child & Adolescent Psychiatry. 2003; 42(2):176–83. doi: 10.1097/00004583-200302000-00011
- Noguera A, Ballesta P, Baeza I, Arango C, de la Serna E, González Pinto A, et al. Twenty four months of antipsychotic treatment in children and adolescents with first psychotic episode. Journal of Clinical Psychopharmacology. 2013; 33(4):463–71. Doi: 10.1097/jcp.0b013e3182962480
- Macmillan I, Howells L, Kale K, Hackmann C, Taylor G, Hill K, et al. Social and symptomatic outcomes of first episode bipolar psychoses in an early intervention service. Early Intervention in Psychiatry. 2007; 1(1):79–87. doi: 10.1111/j.1751-7893.2007.00014.x
- Rabinowitz J, De Smedt G, Harvey PD, Davidson M. Relationship between premorbid functioning and symptom severity as assessed at first episode of psychosis. American Journal of Psychiatry. 2002; 159(12):2021–6. doi: 10.1176/appi.ajp.159.12.2021
- Castro Fornieles J, Parellada M, Gonzalez Pinto A, Moreno D, Graell M, Baeza I, et al. The child and adolescent first episode psychosis study (CAFEPS): Design and baseline results. Schizophrenia Research. 2007; 91(1-3):226–37. doi: 10.1016/j.schres.2006.12.004
- Falcone T, Mishra L, Carlton E, Lee C, Butler R, Janigro D, et al. Suicidal behavior in adolescents with first episode psychosis. Clinical Schizophrenia & Related Psychoses. 2010; 4(1):34–40. doi: 10.3371/csrp.4.1.2
- Chung YC, Jung HY, Kim SW, Lee SH, Shin SE, Shin YM, et al. What factors are related to delayed treatment in individuals at high risk for psychosis. Early Intervention in Psychiatry. 2010; 4(2):124–31. doi: 10.1111/j.1751-7893.2010.00170.x
- Shin YM, Jung HY, Kim SW, Lee SH, Shin SE, Park JI, et al. A descriptive study of pathways to care of high risk for psychosis adolescents in Korea. Early Intervention in Psychiatry. 2010; 4(2):119–23. doi: 10.1111/j.1751-7893.2010.00180.x
- Sharifi V, Kermani Ranjbar T, Amini H, Alaghband Rad J, Salesian N, Seddigh A. Duration of untreated psychosis and pathways to care in patients with first episode psychosis in Iran. Early Intervention in Psychiatry. 2009; 3(2):131–6. doi: 10.1111/j.1751-7893.2009.00119.x
- Archie S, Wilson JH, Woodward K, Hobbs H, Osborne S, McNiven J. Psychotic disorders clinic and first episode psychosis: A program evaluation. The Canadian Journal of Psychiatry. 2005; 50(1):46–51. doi: 10.1177/070674370505000109
- Ballageer T, Malla A, Manchanda R, Takhar J, Haricharan R. Is adolescent onset first episode psychosis different from adult onset. Journal of the American Academy of Child & Adolescent Psychiatry. 2005; 44(8):782–9. doi: 10.1097/01.chi.0000164591.55942.ea
- Marshall M, Lewis S, Lockwood A, Drake R, Jones P, Croudace T. Association between duration of untreated psychosis and outcome in cohorts of first episode patients. Archives of General Psychiatry. 2005; 62(9):975. doi: 10.1001/archpsyc.62.9.975
Type of Study: Original Research |
Subject:
Psychiatry and Psychology
Received: 2016/05/3 | Accepted: 2017/01/25 | Published: 2017/10/1
Received: 2016/05/3 | Accepted: 2017/01/25 | Published: 2017/10/1
References
1. Schimmelmann BG, Conus P, Schacht M, Mcgorry P, Lambert M. Predictors of service disengagement in first admitted adolescents with psychosis. Journal of the American Academy of Child & Adolescent Psychiatry. 2006; 45(8):990–9. doi: 10.1097/01.chi.0000223015.29530.65 [DOI:10.1097/01.chi.0000223015.29530.65]
2. Noguera A, Ballesta P, Baeza I, Arango C, de la Serna E, González Pinto A, et al. Twenty four months of antipsychotic treatment in children and adolescents with first psychotic episode. Journal of Clinical Psychopharmacology. 2013; 33(4):463–71. doi: 10.1097/jcp.0b013e3182962480 [DOI:10.1097/JCP.0b013e3182962480]
3. Castro Fornieles J, Parellada M, Gonzalez Pinto A, Moreno D, Graell M, Baeza I, et al. The child and adolescent first-episode psychosis study (CAFEPS): Design and baseline results. Schizophrenia Research. 2007; 91(1-3):226–37. doi: 10.1016/j.schres.2006.12.004 [DOI:10.1016/j.schres.2006.12.004]
4. Janssen J, Reig S, Parellada M, Moreno D, Graell M, Fraguas D, et al. Regional gray matter volume deficits in adolescents with first-episode psychosis. Journal of the American Academy of Child & Adolescent Psychiatry. 2008; 47(11):1311–20. doi: 10.1097/chi.0b013e318184ff48 [DOI:10.1097/CHI.0b013e318184ff48]
5. Amini H, Alaghbandrad J, Omid A, Sharifi V, Davari Ashtiani R, Momeni F, et al. Diagnostic stability in patients with first-episode psychosis. Australasian Psychiatry. 2005; 13(4):388–92. doi: 10.1111/j.1440-1665.2005.02199.x [DOI:10.1111/j.1440-1665.2005.02199.x]
6. Alaghbandrad J., Amini H., Sharifi V., Dashti B. A 2 year followup study on patients with first episode psychosis admitted to Roozbeh Hospital: Demographic and clinical characteristics and comparison of a specialized program and treatment as usual, Final Report. Tehran: Tehran University of Medical Sciences; 2010.
7. Sharifi V, Amini H, Shahrivar Z, Mottaghipour Y, Mahmoudi Gharaee J, Alaghband Rad J. Courseof psychotic disorders: A 3-year follow up study of patients with first episode psychosis. Iranian Journal of Psychiatry and Clinical Psychology. 2014; 20(1):35-42.
8. Shahrivar Z, Alaghband Rad J, Mahmoudi Gharaie J, Seddigh A, Salesian N, Jalali Roodsari M, et al. The efficacy of an integrated treatment in comparison with treatment as usual in a group of children and adolescents with first episode psychosis during a two year follow up. Iranian Journal of Psychiatry and Clinical Psychology. 2012; 18(2):115-37.
9. Kaufman J, Birmaher B, Brent D, Rao U, Flynn C, Moreci P, et al. Schedule for affective disorders and schizophrenia for school age children-present and lifetime version (K-SADS-PL): Initial reliability and validity data. Journal of the American Academy of Child & Adolescent Psychiatry. 1997; 36(7):980–8. doi: 10.1097/00004583-199707000-00021 [DOI:10.1097/00004583-199707000-00021]
10. Shahrivar Z, Kousha M, Moallemi S, Tehrani Doost M, Alaghband Rad J. The reliability and validity of kiddie schedule for affective disorders and schizophrenia present and life time version - persian version. Child and Adolescent Mental Health. 2010; 15(2):97–102. doi: 10.1111/j.1475-3588.2008.00518.x [DOI:10.1111/j.1475-3588.2008.00518.x]
11. Kay SR, Fiszbein A, Opler LA. The positive and negative syndrome scale (PANSS) for schizophrenia. Schizophrenia Bulletin. 1987; 13(2):261–76. doi: 10.1093/schbul/13.2.261 [DOI:10.1093/schbul/13.2.261]
12. Bates MP. The child and adolescent functional assessment scale (CAFAS): Review and current status. Clinical Child and Family Psychology Review. 2001; 4(1):63-84. [DOI:10.1023/A:1009528727345] [PMID]
13. Patterson DA, Lee MS. Field trial of the Global Assessment of Functioning Scale--Modified. American Journal of Psychiatry. 1995; 152(9):1386–8. doi: 10.1176/ajp.152.9.1386 [DOI:10.1176/ajp.152.9.1386]
14. Shaffer D, Gould MS, Brasic J, Ambrosini P, Fisher P, Bird H, et al. A children's global assessment scale (CGAS). Archives of General psychiatry. 1983; 40(11):1228-31. doi: 10.1001/archpsyc.1983.01790100074010 [DOI:10.1001/archpsyc.1983.01790100074010]
15. Blake K, Cangelosi S, Johnson Brooks S, Belcher HME. Reliability of the GAF and CGAS with children exposed to trauma. Child Abuse & Neglect. 2007; 31(8):909–15. doi: 10.1016/j.chiabu.2006.12.017 [DOI:10.1016/j.chiabu.2006.12.017]
16. World Health Organization. WHOQOL-BREF: Introduction, administration and scoring, Field Trial version. Geneva: World Health Organization; 1996.
17. Nedjat S, Montazeri A, Holakouie K, Mohammad K, Majdzadeh R. Psychometric properties of the Iranian interview-administered version of the World Health Organization's Quality of Life Questionnaire (WHOQOL-BREF): A population based study. BMC Health Services Research. 2008; 8(1):61. doi: 10.1186/1472-6963-8-61 [DOI:10.1186/1472-6963-8-61]
18. Nejat SA, Montazeri A, Holakouie Naieni K, Mohammad KA, Majdzadeh SR. The World Health Organization quality of Life (WHOQOL-BREF) questionnaire: Translation and validation study of the Iranian version. Journal of School of Public Health and Institute of Public Health Research. 2006; 4(4):1-2.
19. Krauss H, Marwinski K, Held T, Rietschel M, Freyberger HJ. Reliability and validity of the Premorbid Adjustment Scale (PAS) in a German sample of schizophrenic and schizoaffective patients. European Archives of Psychiatry and Clinical Neuroscience. 1998; 248(6):277–81. doi: 10.1007/s004060050050 [DOI:10.1007/s004060050050]
20. Brill N, Reichenberg A, Weiser M, Rabinowitz J. Validity of the premorbid adjustment scale. Schizophrenia Bulletin. 2008; 34(5):981–3. doi: 10.1093/schbul/sbm128 [DOI:10.1093/schbul/sbm128]
21. Mahmoodi Gharaei J, Basirnia A, Abedi N, Shadloo B, Jafari S, Salesian N, et al. Association of premorbid adjustment with symptom profile and quality of life in first episode psychosis in a tertiary hospital in Tehran, Iran. Iranian Journal of P sychiatry. 2010; 5(1):23-27. PMCID: PMC3430406 [PMID] [PMCID]
22. Harper A, Power M, Orley J, Herrman H, Schofield H, Murphy B, et al. Development of the World Health Organization WHOQOL-BREF Quality of Life Assessment. Psychological Medicine. 1998; 28(3):551–8. doi: 10.1017/s0033291798006667 [DOI:10.1017/S0033291798006667]
23. Driver DI, Gogtay N, Rapoport JL. Childhood onset schizophrenia and early onset schizophrenia spectrum disorders. Child and Adolescent Psychiatric Clinics of North America. 2013; 22(4):539–55. doi: 10.1016/j.chc.2013.04.001 [DOI:10.1016/j.chc.2013.04.001]
24. Schreier HA. Hallucinations in nonpsychotic children: More Common than we think. Journal of the American Academy of Child & Adolescent Psychiatry. 1999; 38(5):623–5. doi: 10.1097/00004583-199905000-00028 [DOI:10.1097/00004583-199905000-00028]
25. Jarbin H., Ott Y., Von Knorring AL. Adult outcome of social function in adolescent onset schizophrenia and affective psychosis. Journal of the American Academy of Child & Adolescent Psychiatry. 2003; 42(2):176–83. doi: 10.1097/00004583-200302000-00011 [DOI:10.1097/00004583-200302000-00011]
26. Noguera A, Ballesta P, Baeza I, Arango C, de la Serna E, González Pinto A, et al. Twenty four months of antipsychotic treatment in children and adolescents with first psychotic episode. Journal of Clinical Psychopharmacology. 2013; 33(4):463–71. Doi: 10.1097/jcp.0b013e3182962480 [DOI:10.1097/JCP.0b013e3182962480]
27. Macmillan I, Howells L, Kale K, Hackmann C, Taylor G, Hill K, et al. Social and symptomatic outcomes of first episode bipolar psychoses in an early intervention service. Early Intervention in Psychiatry. 2007; 1(1):79–87. doi: 10.1111/j.1751-7893.2007.00014.x [DOI:10.1111/j.1751-7893.2007.00014.x]
28. Rabinowitz J, De Smedt G, Harvey PD, Davidson M. Relationship between premorbid functioning and symptom severity as assessed at first episode of psychosis. American Journal of Psychiatry. 2002; 159(12):2021–6. doi: 10.1176/appi.ajp.159.12.2021 [DOI:10.1176/appi.ajp.159.12.2021]
29. Castro Fornieles J, Parellada M, Gonzalez Pinto A, Moreno D, Graell M, Baeza I, et al. The child and adolescent first episode psychosis study (CAFEPS): Design and baseline results. Schizophrenia Research. 2007; 91(1-3):226–37. doi: 10.1016/j.schres.2006.12.004 [DOI:10.1016/j.schres.2006.12.004]
30. Falcone T, Mishra L, Carlton E, Lee C, Butler R, Janigro D, et al. Suicidal behavior in adolescents with first episode psychosis. Clinical Schizophrenia & Related Psychoses. 2010; 4(1):34–40. doi: 10.3371/csrp.4.1.2 [DOI:10.3371/CSRP.4.1.2]
31. Chung YC, Jung HY, Kim SW, Lee SH, Shin SE, Shin YM, et al. What factors are related to delayed treatment in individuals at high risk for psychosis. Early Intervention in Psychiatry. 2010; 4(2):124–31. doi: 10.1111/j.1751-7893.2010.00170.x [DOI:10.1111/j.1751-7893.2010.00170.x]
32. Shin YM, Jung HY, Kim SW, Lee SH, Shin SE, Park JI, et al. A descriptive study of pathways to care of high risk for psychosis adolescents in Korea. Early Intervention in Psychiatry. 2010; 4(2):119–23. doi: 10.1111/j.1751-7893.2010.00180.x [DOI:10.1111/j.1751-7893.2010.00180.x]
33. Sharifi V, Kermani Ranjbar T, Amini H, Alaghband Rad J, Salesian N, Seddigh A. Duration of untreated psychosis and pathways to care in patients with first episode psychosis in Iran. Early Intervention in Psychiatry. 2009; 3(2):131–6. doi: 10.1111/j.1751-7893.2009.00119.x [DOI:10.1111/j.1751-7893.2009.00119.x]
34. Archie S, Wilson JH, Woodward K, Hobbs H, Osborne S, McNiven J. Psychotic disorders clinic and first episode psychosis: A program evaluation. The Canadian Journal of Psychiatry. 2005; 50(1):46–51. doi: 10.1177/070674370505000109 [DOI:10.1177/070674370505000109]
35. Ballageer T, Malla A, Manchanda R, Takhar J, Haricharan R. Is adolescent onset first episode psychosis different from adult onset. Journal of the American Academy of Child & Adolescent Psychiatry. 2005; 44(8):782–9. doi: 10.1097/01.chi.0000164591.55942.ea [DOI:10.1097/01.chi.0000164591.55942.ea]
36. Marshall M, Lewis S, Lockwood A, Drake R, Jones P, Croudace T. Association between duration of untreated psychosis and outcome in cohorts of first episode patients. Archives of General Psychiatry. 2005; 62(9):975. doi: 10.1001/archpsyc.62.9.975 [DOI:10.1001/archpsyc.62.9.975]
| Rights and permissions | |
 |
This work is licensed under a Creative Commons Attribution-NonCommercial 4.0 International License. |